We are a multidisciplinary team within LSHTM. We are also part of the CGIAR Research Program on Agriculture for Nutrition and Health (A4NH) supported by the CGIAR, a global consortium of donors and research centres for agricultural development. We work with a range of CGIAR centres, including the International Livestock Research Institute (ILRI), the International Food Policy Research Institute (IFPRI), the International Institute for Tropical Agriculture (IITA), International Rice Research Institute (IRRI) and AfricaRice.
We co-manage one of A4NH’s research programmes called Improving Human Health (IHH), which addresses the side-effects of agriculture on infectious disease. Our research is focused on agricultural landscapes and vector-borne disease, emerging and neglected zoonotic diseases, and antimicrobial resistance.
Our programme with A4NH is part of a broader LSHTM research collaboration with A4NH and other institutions on agriculture, food systems and health.
The LSHTM Agriculture and Infectious Disease group studies the effects of changing agricultural and food systems on human infectious diseases. Agriculture and the food systems that it supports are essential for human health, but sometimes agricultural activities and environments can generate unintended health side-effects.
For example, farm landscapes can create vector breeding sites or promote vector contact, while livestock food chains can promote the transmission of zoonotic diseases between humans and animals, and contribute to antibiotic resistance in human pathogens.
Our aim is to develop and promote agricultural methods that are safe for human health. This also contributes to the sustainability of agriculture and food systems, food security and nutrition.
Our research programme complements and supports the Agriculture for Nutrition and Health (A4NH) programme run by CGIAR, a global consortium of donors and research centres for agricultural development.
The A4NH programme brings together researchers in CGIAR research centres and universities around the globe to conduct innovative research to make agricultural production, food system and diets in low- and middle-income countries more sustainable, nutritious and healthy.
With International Livestock Research Institute (ILRI), we co-manage one of A4NH’s research flagships called Improving Human Health (IHH), which addresses the side-effects of agriculture on infectious disease. We also work with a range of other CGIAR centres, including the International Food Policy Research Institute (IFPRI), the International Institute for Tropical Agriculture (IITA), International Rice Research Institute (IRRI) and AfricaRice.
As one of the A4NH managing partners, we also facilitate links between LSHTM programmes in agriculture, nutrition and health and other research groups in the A4NH programme working on food systems for healthier diets, micronutrient biofortification of crops, policies and programmes for improved nutrition, and food safety.
Within the A4NH Improving Human Health (IHH) flagship programme, there are three clusters of research, concerned with:
- Diseases in agricultural landscapes
- Emerging and neglected zoonotic diseases
- Global challenges in agriculture and health
You can read more about these areas in CGIAR's Strategic Brief.
Our LSHTM group focuses particularly on the first and last. For agricultural landscapes, our current research focuses on the relationship between rice production and malaria. Under global challenges for agriculture and health, our current work focuses on anti-microbial resistance. We also facilitate A4NH links on zoonotic disease research with LSHTM colleagues and with our partners at the Royal Veterinary College.
Recently the CGIAR has added a new IHH activity, a global COVID-19 Hub, and LSHTM has a key partnership role in that as well, which we facilitate.
Rice and malaria
Agriculture is the main driver of environmental change in rural settings. Landscapes that are 100% man-made are becoming more common in rural settings in tropical countries, and agricultural landscapes are growing features in urban areas. Compared to other infections, vector-borne diseases are especially vulnerable to environmental change because transmission is sensitive to any factor that may alter the behaviour and ecology of the vector.
A key challenge today is the intensification of rice in Africa and its potential impact on malaria elimination there. Mosquitoes breed in rice fields everywhere, but this is a particular problem in Africa because the main ricefield-breeding mosquito species is Anopheles gambiae. This is the main vector of malaria in Africa and its efficiency in transmitting the parasite is the main reason why more than 85% of world’s deaths due to malaria are suffered by in African children.
Our research with African agricultural and health research groups will develop ways to grow more rice without growing more malaria. Our partners at the International Livestock Research Institute (ILRI) also work on landscape aspects of other vector-borne diseases like Rift Valley Fever, Japanese Encephalitis and Dengue.
Other collaborating research partners include AfricaRice, the International Institute of Tropical Agriculture (IITA), the International Rice Research Institute (IRRI), Institut Pierre Richet (IPR) and and Ifakara Health Institute.
We are currently focused on the following projects:
- Re-assessing ‘paddies paradox’: how rice and malaria are linked in Africa
-
Rice-growing villages in Africa have very high densities of malaria vectors, but do these extra mosquitoes also bring more malaria? When this question was reviewed two decades ago, the answer was ‘surprisingly not’. This was mainly because rice also brought socioeconomic benefits, which meant people could afford better protection, such as mosquito nets. Since then, however, greater and more equitable protection measures have significantly reduced malaria transmission across the continent.
Kallista Chan and Jo Lines conducted a meta-analysis of previous and more recent studies into whether the ‘paddies paradox’ still holds true. They found that mosquito numbers were not only (up to 8-fold) higher in irrigated rice farming villages than non-rice farming villages, but that since 2003, malaria prevalence was almost 2-fold higher too.
- Anopheles mosquito control in Africa: the effect of rice cultivation practices
-
In order to continue increasing rice production in Africa, without increasing the burden of malaria, we need a better understanding of how different rice-growing techniques affect the reproduction of mosquitoes. Kallista Chan is conducting a systematic review to identify methods of rice cultivation that may be effective in reducing the number of malaria vectors. This will also include mosquito larvae control methods, such as introducing fish or the bacterium Bacillus thuringiensis israelensis, intermittent irrigation and plant variety. Experimental fields are also being established, in collaboration with AfricaRice and the International Rice Research Institute, to measure the effect of new rice cultivation practices (e.g. alternate wetting and drying irrigation) on mosquitoes.
- Determining the malaria vector productivity of rice fields
-
Kallista Chan is developing an effective and representative sampling method for monitoring mosquito numbers in rice fields, that could be incorporated into routine rice research. Kallista is trialling different methods of sampling mosquitoes in Côte d’Ivoire (such as standard dipping and adult emergence traps) and assessing their effectiveness by comparing sampled numbers with absolute numbers collected via area samplers. An accurate, standardised method to measure the number of mosquitoes breeding in rice fields will be vital to understand the extent of the rice-malaria problem and to enable future research into rice-growing techniques.
- Rice farmers’ views and perspectives on rice farming and its effect on mosquitoes
-
The compliance of farmers will be essential to successfully implement new rice-growing techniques that reduce mosquito productivity. However, anecdotal evidence suggests that their motives to adopt new technologies seem to fundamentally involve economic benefits, rather than mosquito nuisance or health.
These observations solicit questions on how rice farmers feel towards mosquitoes, how they view themselves in the production of mosquitoes, what would motivate them to change their rice-growing practices and how they could cooperate to implement collective vector control. In collaboration with Institut Pierre Richet and Universite Alassane Ouattara in Cote d’Ivoire, Kallista Chan is conducting semi-directed, in-depth interviews to understand farmers’ experiences, perceptions, motivations and values regarding mosquitoes as well as focus-group discussions to analyse the capacity of rice-growing communities to collectively search for a solution to reduce mosquito production.
- Using Earth Observation data to identify vector habitats in agricultural landscapes
-
Understanding how agricultural practices affect mosquito density and disease transmission is vital to the sustainable management of landscapes to improve public health. In a project led by Dr Kimberly Fornace at LSHTM, in partnership with the Health Innovation Laboratory at the Universidad Peruana Cayetano Heredia in Peru, we’re using Earth Observation data and advances in artificial intelligence to study these interactions. We’re integrating data on land-use, collected from drone flights and satellite imagery, with ground-based observations of mosquito larvae habitats and adult mosquito densities, and developing new deep learning algorithms that can identify mosquito habitats in agricultural landscapes.
Outputs:
- Achieving global malaria eradication in changing landscapes. Fornace, K.M., Diaz, A.V., Lines, J. et al. Malar J 20, 69 (2021).
- Technical Workflow Development for Integrating Drone Surveys and Entomological Sampling to Characterise Aquatic Larval Habitats of Anopheles funestus in Agricultural Landscapes in Côte d’Ivoire. Byrne I., Chan K., Lines J., Cook J., N'Guessan R., Messenger L., Kristan M., Fornace, K. et al. Journal of Environmental and Public Health.
Anti-microbial resistance (AMR) from a One Health perspective
The A4NH IHH research cluster on Global Challenges in Agriculture and Health addresses problems common to agriculture and health where an integrated approach may be more effective than separate sectoral interventions. These include tacking AMR, where agricultural use, largely in livestock and fish production may create risks for humans, and resistance to insecticides, where insecticide use in agricultural pest management and disease vector control in LMICs may come into conflict.
Our work focuses on AMR, where we lead and collaborate on a number of projects in Africa and Asia. LSHTM is also the managing partner of the new CGIAR AMR Hub, which applies a One Health approach to support the efforts of LMICs in controlling agriculture-associated AMR risks, through promoting and facilitating trans-disciplinary partnerships.
Working together with ILRI, the Royal Veterinary College and national partners in Africa and Asia, we have the following portfolio of current research projects:
- WASH and structural interventions to reduce antimicrobial resistance
-
Chris Pinto, Sarai Keestra and Clare Chandler researched how water, sanitation and hygiene (WASH) and biosecurity interventions could reduce infections, antimicrobial use and antimicrobial resistance (AMR) in people working in close contact with animals, such as farmers. This project considered different settings, with a focus on low- and middle-income countries. Previous research suggested that social, cultural, political, economic and environmental factors play an important role in the development of AMR, however, it was not well-understood how these effects can be mitigated. This systematic review, in collaboration with the LSHTM AMR Centre and the International Livestock Research Institute (ILRI), summarised the evidence base for such structural AMR interventions, with the aim of shaping future research, policies and funding in this area.
See the research protocol for more information.
A total of 104 studies were included in the review, which identified a number of effective interventions to reduce the burden of infections, antimicrobial resistance and antibiotic use in animal agricultural settings. Interventions which undertook biomanagement and bio-containment measures appeared to have positive effects most often. These measures attempted to create and maintain a conducive environment for animal raising in terms of physical infrastructure and protocols. The few studies reporting sanitation measures - which were similar to bio-containment interventions - all reported positive effects. By contrast, efforts to impact water quantity, water quality, and hygiene had more mixed effects on the outcomes assessed. Bio-exclusion interventions had mostly negative effects.
However, risk of bias was high or moderate in many studies, and publication bias should also be considered. These findings demonstrate the need for more, high-quality studies evaluating structural interventions. There are opportunities to learn from biosecurity Interventions for WASH and the authors propose that the 'A' In WASH represents both 'Animals' and 'Air', in recognition of these infection pathways.
Outputs:
- WASH and biosecurity interventions for reducing burdens of infection, antibiotic use and antimicrobial resistance in animal agricultural settings: a One Health mixed methods systematic review. Pinto C. J., Keestra, S., Tandon, P., Chandler, C.I.R. LSHTM Project Report, 2020.
- Health risks and transmission pathways associated with antimicrobial use in crops
-
Ariel Brunn and Jeff Waage are conducting a literature review of the potential health risks and transmission pathways associated with antimicrobial use in crop production, with a focus on low- and middle-income countries (LMICs). Crops are treated with protective antimicrobials and biocides, which may select for drug-resistant microbes either on the crops or in the human body after ingestion. These resistant microbes can also persist in soil, manure and irrigation water, leading to further spread. The evidence supporting transmission pathways for AMR through crop production and its value chains is limited, particularly for LMICs. Risk factors in these countries are different due to closer integration of crop and livestock production, agricultural contamination of water sources, challenges with local sanitation and hygiene, and limited resources for national surveillance and response.
- Uncovering the history of antibiotic use in Africa
-
Paula Palanco researched one of the gaps existing in the history of drugs: the arrival and generalisation of the use of antibiotics in African settings. Taking into account the expansionist colonial interests of European powers, this project looked beyond the fatalistic stories about self-medication, irrational use and abuse by African people, looking at the context and the conditions in which antibiotics were first used in these locations. For this, this project aimed to provide a nuanced account of when, how and why antibiotics arrived in three different locations: Zimbabwe, Malawi and Uganda.
Output:
- Histories of Antibiotics: A One Health account of the arrival of antimicrobial drugs to Zimbabwe, Malawi and Uganda. Palanco Lopez, P., Chandler, C.I.R. LSHTM Project Report, 2020.
- Developing online health economics tools for One Health researchers
-
Nichola Naylor is developing a combined cost-utility and cost-benefit model of AMR interventions, across agriculture and human healthcare systems, that can be adapted to different settings. This open-access code will be shared online, to accelerate research in this field around the world. She has also already launched an online tool called Signposting Health Economic Packages in R for Decision Modelling (SHEPRD). The site aims to help you navigate you through the forest of R packages that can be used in health economics and signpost you to the most appropriate one, given your intended analysis.
- Improving methods for evaluating the cross-sectoral impact of health interventions
-
Nichola Naylor is developing a new modelling approach to better evaluate the effectiveness of health interventions, such as those intended to reduce antimicrobial resistance. Her method with integrate cross-sectoral metrics to evaluate the impact of a particular intervention on humans, animals and the environment. The outcomes of this model can then feed into decision analyses that weigh respective impact estimates alongside other considerations, such as equity or uncertainty. This approach will give policymakers a clearer understanding of the ‘One Health’ impact of health interventions, leading to better evidence-based decision-making.
Outputs:
- Quantitatively evaluating the cross-sectoral and One Health impact of interventions: A scoping review and case study of antimicrobial resistance. N. R. Naylor, J. Lines, J. Waage, B. Wieland, G. M. Knight, One Health, 11 (2020).
- Download a PDF infographic.
- Quantitatively evaluating the cross-sectoral and One Health impact of interventions: A scoping review and case study of antimicrobial resistance. N. R. Naylor, J. Lines, J. Waage, B. Wieland, G. M. Knight, One Health, 11 (2020).
- Understanding the impact of antibiotic resistance on quality of life
-
While the effect of antibiotic resistance on the incidence and mortality of disease is increasingly well-understood, the impact it has on individuals’ quality of life – through cases of untreatable chronic illnesses – has been less widely studied. Nichola Naylor is leading a literature review looking at how antibiotic resistance impacts disease burden, taking into account health-related quality of life as well as years lived, to assess the existing evidence in this field.
- Understanding the economic impact of antibiotic resistance
-
Nichola Naylor is working with the World Health Organisation to evaluate the economic cost of antibiotic resistance in different settings. This research will look at factors such as increased healthcare costs and decreased labour productivity arising from a greater burden of disease, and will include literature reviews, meta-analyses and modelling approaches.
Other projects
- Using Earth Observation data to predict Rift Valley Fever outbreaks
-
Kimberley Fornace and Stephanie Key are analysing Earth Observation (EO) data derived from aerial drone and satellite imagery to study the influence of fine-scale landscape features on Rift Valley Fever (RVF) transmission.
RVF is a viral mosquito-borne zoonosis. Though it primarily affects animals, humans can also contract the disease, usually through contact with infected livestock.
Drones can be used to conduct in-depth investigations of environmental factors leading to RVF outbreaks, allowing monitoring of changes at fine spatial and temporal scales which would not be possible through satellite data due to frequent cloud cover and revisiting times. Additionally, drones can be used to collect data on the distributions and densities of wildlife and livestock disease reservoirs.
This project will incorporate citizen science activities for the identification of animals from drone data, via the Zooniverse platform, and explore how new sources of EO data, citizen science involvement, and computational advances in machine learning can be used to characterise RVF virus transmission and develop more accurate risk maps.
The data used has been collected as part of a larger ILRI project: Co-infection with Rift Valley fever virus, Brucella spp and Coxiella burnetti in humans and animals in Kenya: disease burden and ecological factors.

Jeff Waage
PROFESSOR
Kimberley Fornace
ASSISTANT PROFESSOR

Maria Bernardez
RESEARCH PROGRAMME MANAGER
External partners
From ILRI (Kenya)
Dr. Delia Randolph; Dr. Bernard Bett; Dr. Barbara Wieland; Prof. Eric Fevre (from ILRI but also from University of Liverpool); Mrs. Stella Ikileng; Ms. Wacera Ngonga; Ms. Victoria Kyallo
From ILRI (Vietnam)
Dr. Joanna Lindahl; Dr. Hung Nguyen; Dr. Fred Unger; Dr. Hu Suk Lee
From IITA
Dr. Rousseau Djouaka; George Mahuku; Joshua Adeoye
From Africa Rice
Dr. Saito Kazuki; Dr. Elliot Dossou-Yovo; Mr. Salifou Goube-Mairoua; Mr. Mazen El Solh
From IPR
Dr. Raphael N’Guessan; Dr. Alphosine Koffi; Dr. Dimi Doudou; Mr. Lucien You Bi
From IRRI
Dr. Abdelbagi Ismail; Mr. George Iranga
From IHI
Dr. Sarah Moore, Ms. Edith Madumla, Mr. Mgeni Mohamed
From ITM
Dr. Koen Peeters Grietens; Dr. Maya Ronse; Dr. Thuan thi Nguyen
From RVC
Dr. Pablo Alarcon Lopez; Dr. Ana Mateus; Mr. Mathew Hennessey
From IFPRI
Dr. John McDermott; Ms. Amanda Wyatt; Mrs. Tigist Defabachew; Mrs. Janet Hudor; Ms. Elena Martinez
From LSHTM
Dr. Clare Chandler; Dr. Sian Clarke; Dr. Richard Stabler; Dr. Paula Dominguez-Salas; Dr. Harparkash Kaur; Dr. Gwen Knight; Ms. Jenny Westad
New research appears to reverse the ‘paddies paradox’ and highlights a need to improve methods for growing rice in sub-Saharan Africa without increasing the number of mosquitoes.
MSc student Dina Youssef performed the first systematic analysis of the impact of farm-level biosecurity interventions on reducing the spread of disease from animals to humans, recently published in Zoonoses and Public Health.
14 studies were analysed that covered a range of measures including handwashing, sanitisation and hygienic measures, personal protective equipment (PPE), vaccination and changes to routine farm activities.
A mixed picture emerged from the results; while the majority of studies did indicate that biosecurity measures reduced bacteria transmission to farmers, there were some studies that found no statistically robust evidence of benefit. Importantly, the review highlighted the lack of research in this area, with few large, comprehensive studies available.
- To find out more, you can read read our blog or the access the full paper.
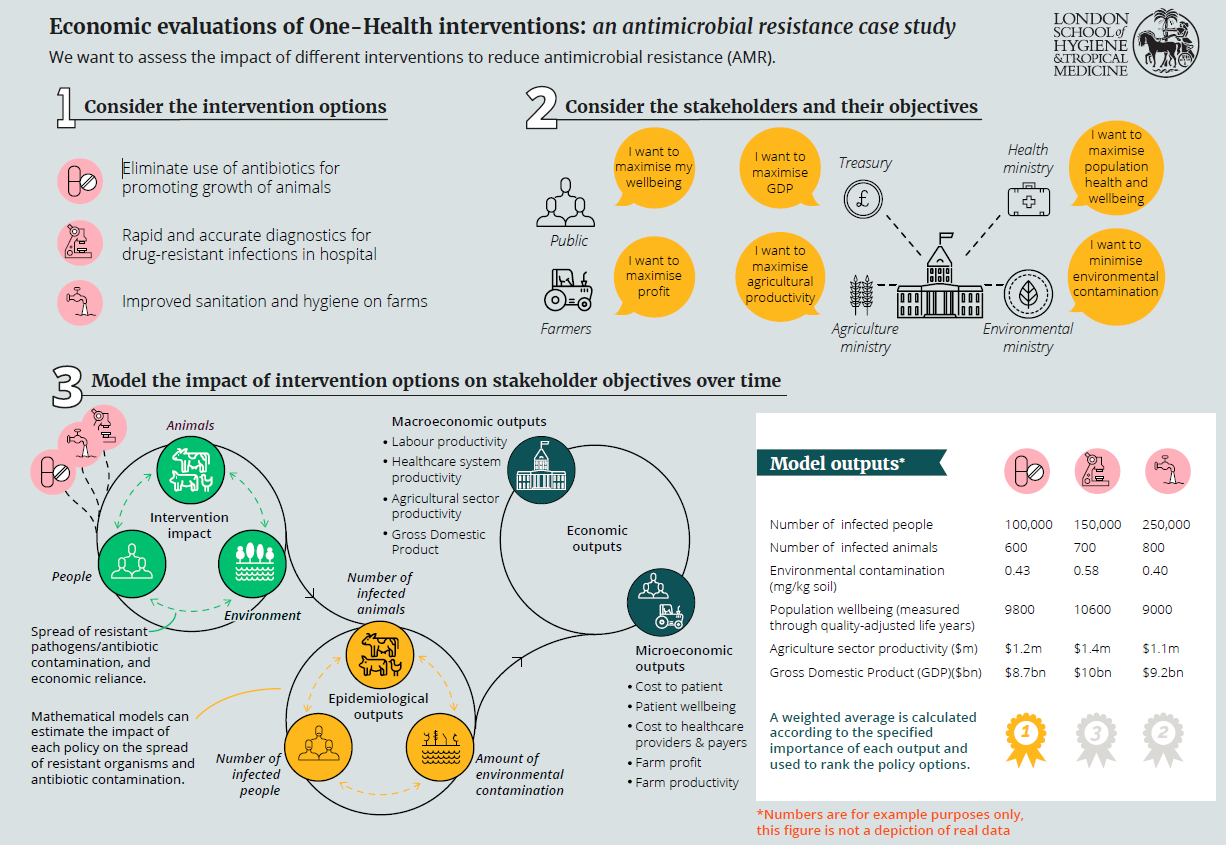
We've published a new paper in the journal One Health, led by Dr Nichola Naylor, that sets out a method of quantitatively evaluating the impact of health interventions. This method is designed to analyse interventions related to One-Health, i.e. those that affect different sectors including humans, animals and the environment.
The study reviewed 90 different papers describing a range of different modelling techniques, and this information informed the construction of this new approach.
The proposed method was applied to an antimicrobial resistance (AMR) case study. AMR is a typical One-Health issue, with microbes moving between people, farm animals and the environment, such as soil and water.
The study highlights the need to consider different stakeholder objectives - in this case, the aims of the public, farmers and different government ministries, in order to establish the optimal course of action to tackle complex health issues.
LSHTM has recently launched the second season of its podcast, LSHTM Viral. This series focuses on planetary health, featuring researchers from LSHTM's newly formed Centre on Climate Change & Planetary Health.
Episode 4 deep dives into how environmental changes can affect infectious diseases, with Kallista Chan discussing the Agriculture and Infectious Disease Group's research on rice cultivation and malaria.
You can listen to LSHTM Viral wherever you get your podcasts: Anchor, Apple Podcasts, Breaker, Castbox, Google Podcasts, Spotify, Stitcher.
We've published our strategic brief for 2020, co-authored with our partners at ILRI and CGIAR, which highlights the key health risks associated with agricultural intensification. These include:
- Environmental changes associated with development of agricultural landscapes, for example, an increase in malarial mosquitoes caused by expanding rice fields.
- The transfer to humans of pathogens and toxins during agricultural production processes and via food value chains, as most recently seen with COVID-19.
- Interference between parallel agricultural and health interventions, such as increasing antimicrobial resistance.
Human health is a fundamental feature of sustainable agricultural intensification. Cross-sectoral collaboration, involving public health as well as agricultural research institutions, is needed to support basic research and the development and implementation of interventions.
As the impacts of COVID-19 spread across the globe, the virus threatens more than health systems worldwide. It also poses serious risks to food security, local businesses and national economies, and hard-fought progress by stakeholders at all levels towards the Sustainable Development Goals.
LSHTM joins the International Food Policy Research Institute (IFPRI), the International Livestock Research Institute (ILRI), and the CGIAR System Organization as co-implementers of a new COVID-19 Hub to consolidate existing scientific evidence and help support response, recovery and resilience measures in the face of the coronavirus pandemic.
In 2019, Joanna Kuper completed an MSc in Public Health for Development at LSHTM. Her summer research project focused on human/animal ‘crossover-use’ of antibiotics in Uganda. In this article, Joanna recounts some of her experience and research findings.
Antimicrobial resistance (AMR) has been described as the ‘quintessential’ One Health issue. Yet there are significant gaps in our knowledge, in particular in many low- and middle-income countries (LMICs).
In 2019, aided by generous funding from CGIAR, I went to Luwero district, Uganda to carry out a qualitative study into ‘crossover-use'. By this I mean people treating animals using human medicines or treating themselves using veterinary medicines, with a focus on antibiotics.
I was following in the footsteps of previous MSc students who visited Luwero district in 2018, where they heard accounts of farmers giving human medicines to chickens and pigs, and of people using veterinary drugs to treat themselves for wounds or sexually transmitted infections (STIs).
On 18 March 2020 the LSHTM, in collaboration with the CGIAR A4NH research programme, hosted the Antibiotic Resistance-related Intervention Impact Evaluation workshop.
This virtual workshop brought together epidemiologists and economists across the One Health system to discuss methods of evaluating disease burden and the impact of interventions in relation to antibiotic resistance.
We covered mathematical, statistical and economic modelling methods used by esteemed colleagues across numerous institutions. Commonalities across the different methods were highlighted; namely a need for more data.
This session also offers insight into potential ways to integrate and share model inputs, outputs and code within this field.
Nichola Naylor, research fellow in the Agriculture and Infectious Disease group has launched an online tool called Signposting Health Economic Packages in R for Decision Modelling (SHEPRD).
The site aims to help you navigate you through the forest of R packages that can be used in health economics and signpost you to the most appropriate one, given your intended health economic analysis.
This decision tree-style compendium was created over 2 days as part of a R Hackathon (6th - 7th November 2019), with work continued until 2020. The R Hackathon was organised by Dr Nathan Green and Imperial College London.
Last November, Wellcome launched the Wellcome Data Re-use Prize for AMR surveillance as a challenge for teams around the world to 'generate a new insight, tool or health application' from data held in the AMR Research Initiative - a partnership between the Open Data Institute and the Wellcome Trust.
We are pleased to announce that Nichola Naylor, research fellow in the Agriculture and Infectious Disease group, won first prize as part of the Antibiotic Resistance: Interdisciplinary Action (AR:IA) team, along with Gwen Knight, Francesc Coll, Quentin Leclerc, and Alex Aiken.
The team developed an interactive web app that lets users quickly visualise resistance rates to antibiotics for common infections and countries of interest. The data on the platform will help doctors to prescribe more appropriately in the face of local drug-resistance.
- For more information, you can read their report or try out their app.
Our programme with A4NH is part of a broader LSHTM research collaboration with A4NH and other institutions on agriculture, food systems and health.
We work closely with ongoing LSHTM programmes on nutrition including Improving Metric and Methods for Agriculture-Nutrition Action (IMMANA) and Sustainable and Healthy Food Systems (SHEFS). With IMMANA, A4NH contributes to the Agriculture, Nutrition and Health (ANH) Academy with a membership of 2000+ research scientists in 90+ countries and 700+ institutions, mostly in LMICs.
These and other LSHTM projects are all partners with us in the London Centre for Integrative Research on Agriculture and Health (LCIRAH) which has provided for almost a decade a monthly platform for interdisciplinary dialogue on agriculture and health research collaboration between LSHTM, SOAS, RVC and City University.
We encourage anyone at LSHTM interested in health links with agriculture to contact LCIRAH.