Carbapenem-resistant Acinetobacter baumannii (CRAB) is an opportunistic bacterial pathogen that causes infections in hospitalised patients and those with critical illness. To make matters worse, CRAB exhibits a tendency to rapidly accumulate resistance mechanism to multiple antibiotic classes, rendering once-preferred treatment obsolete. It is no surprise that the World Health Organisation has listed CRAB is as a “priority 1: Critical” pathogen to develop new antibiotics against1.
What are Carbapenems, the antibiotics to which this nasty pathogen is resistant to?
Carbapenems belong to a subclass of antibiotics class called β- lactam antibiotics. This class also includes the well-known penicillins and cephalosporins. What distinguishes carbapenems is that they are reserved for treating severe illness, and must be given intra-venously in hospital. However, the misuse of carbapenems has led to emergence of carbapenem-resistant bacteria. With the options beyond carbapenems scarce, the hope for a novel class of antibiotics substantially increases.
For more than half a century, no new antibiotic class against A. baumannii has reached patients. As we exhaust available antibiotic classes, novel classes against previously “undruggable” targets becomes dire. To address this, scientists employed high-throughput approach to screen a library of 44,985 compounds against a collection of bacterial pathogens. The results showed a compound, R07036668, to be active against A. baumannii. This finding prompted the further enhancement of the compound, resulting in the first-generation lead compound, R07075573. When tested in laboratory animals, R07075573 was found to protect mice from infections due to CRAB. Subsequent modifications were performed on the compound to improve its safety profile and clinical compatibility, leading to the second-generation lead, zosurabalpin2.
What is new then about Zosurabalpin’s mode of action?
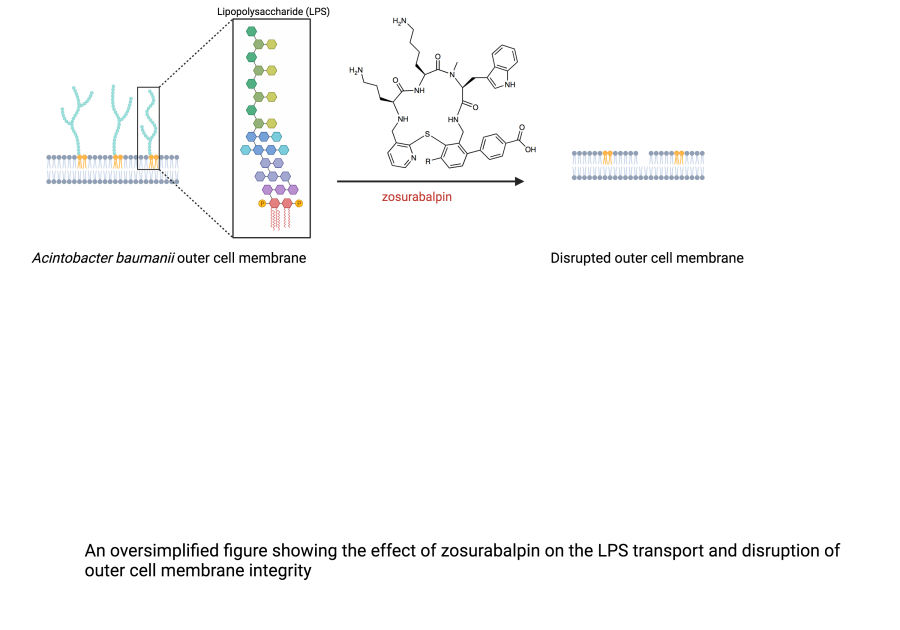
The outer cell envelope of Acinetobacter baumannii and other Gram-negative bacteria is composed of a large molecule called lipopolysaccharide (LPS) making it impenetrable. The process through which LPS is transported to the outer cell envelope is critical for the cell integrity and essential for bacterial cell viability. The promising drug zosurabalpin inhibits LPS transport, and subsequently disrupts the bacterial envelope integrity3.
Is Zosurabalpin considered a magic bullet?
Yes, and no. The breakthrough nature of this work stems from the fact that LPS transport mechanism has not been successfully targeted before, which opens the door for more studies to improve compounds activities of this class. However, resistance might emerge to this new class of antibiotics. To mitigate emerging resistance to zosurabalpin, antibiotic combinations might be used to treat CRAB infections.
This is an important step to combat a pathogen that has accumulated an extensive molecular arsenal against all antibiotics currently available in the clinic.
References:
2- Zampaloni, C., Mattei, P., Bleicher, K. et al. A novel antibiotic class targeting the lipopolysaccharide transporter. Nature 625, 566–571 (2024). https://doi.org/10.1038/s41586-023-06873-0
3- Pahil, K.S., Gilman, M.S.A., Baidin, V. et al. A new antibiotic traps lipopolysaccharide in its intermembrane transporter. Nature 625, 572–577 (2024). https://doi.org/10.1038/s41586-023-06799-7
LSHTM's short courses provide opportunities to study specialised topics across a broad range of public and global health fields. From AMR to vaccines, travel medicine to clinical trials, and modelling to malaria, refresh your skills and join one of our short courses today.
