We aim to address the urgent need for improving control of non-communicable diseases (NCDs) in West Africa, where healthcare has been traditionally neglected and driven by disease-specific programmes, with limited engagement of local communities.
Our partnership is led by the London School of Hygiene and Tropical Medicine (LSHTM) and Ghana College of Physicians and Surgeons (GCPS), and involves Ashesi University (AU), Laboratoire d'Etudes et de Recherche sur les Dynamiques Sociales et le Développement Local [Research Laboratory on Social Dynamics and Local Development] (LASDEL) and Université Catholique de l'Afrique de l'Ouest - Unité Universitaire at Bobo-Dioulasso [Catholic University of West Africa - University Unit at Bobo-Dioulasso] (UCAO-UUB).
STOP-NCD is a NIHR Global Health Research Centre for non-communicable diseases in West Africa (STOP-NCD) funded by the NIHR and hosted by LSHTM and GCPS.
Funded by the National Institute for Health and Care Research (NIHR), between 2022 and 2027, the NIHR Global Health Research Centre for Non-communicable Disease Control in West Africa (Stop-NCD) project is a partnership between the Ghana College of Physicians and Surgeons, the London School of Hygiene & Tropical Medicine, Ashesi University, Laboratoire d'Etudes et de Recherche sur les Dynamiques Sociales et le Développement Local [Research Laboratory on Social Dynamics and Local Development] (LASDEL) and Université Catholique de l'Afrique de l'Ouest - Unité Universitaire at Bobo-Dioulasso [Catholic University of West Africa - University Unit at Bobo-Dioulasso] (UCAO-UUB). We will use comprehensive and sustainable approaches to capacity strengthening, improving individual, organisational and system-level capacities of:
- researchers, particularly earlier-career staff, for high-quality applied NCD research,
- local communities, to engage with and improve behaviours and decisions affecting their health and
- policymakers and practitioners, to implement evidence-based NCD interventions.
We aim to improve health and wellbeing of populations in West Africa by developing capacity for high-quality research to inform improved prevention, diagnosis and treatment of inter-connected NCDs (hypertension, diabetes and co-existing stress, anxiety and depression).
To do this we will:
- Work in three West African countries (Ghana, Burkina Faso and Niger) with varying ethnic, social, cultural and economic environments to develop, implement and evaluate ways of improving control of hypertension, diabetes and related stress, anxiety and depression.
- We will start by analysing roles of key stakeholders (patients and communities, health workers, managers, policymakers) in the development, provision and use of NCD policies, programmes and services in each country, using appropriate methods such as analysis of available data, observations and interviews;
- Working closely with those stakeholders, we will co-produce packages of interventions for improving NCD control. This package will include adapting international guidelines to local contexts and supporting healthcare workers in implementing these, and establishing a community-based prevention, early-detection and management of NCDs;
- We will implement and rigorously evaluate the interventions packages for their costs and effectiveness, assess their potential for wide-scale application, and will identify transferable lessons for improving NCD control beyond these three countries.
Throughout these steps, we will strengthen individual skills and expertise, organisational systems and processes and system-wide networking capabilities and leadership of:
- researchers (to conduct high-quality research),
- local communities (to engage with, and understand, how to enable healthy lifestyles) and
- policymakers and practitioners (to implement evidence-based NCD interventions)
London School of Hygiene & Tropical Medicine (joint lead organisation)
- Prof Tolib Mirzoev
- Prof Martin McKee
- Prof Dina Balabanova
- Prof Pablo Perel
- Dr Eleanor Hutchinson
- Dr Neil Spicer
- Dr Adrianna Murphy
- Dr Yasmin Jahan
- Dr Diane Duclos
- Miss Veronika Reichenberger
- Peta-Ann King
- Ayan Aden Hag Hersi
Website: www.lshtm.ac.uk.
Ghana College of Physicians and Surgeons (joint lead organisation)
- Prof Irene Agyepong
- Prof Evelyn Ansah
- Dr Abraham Oduro
- Dr Mary Amoakoh Coleman
- Dr Jacob Nonvignon
- Dr Augustina Koduah
- Dr Edward Antwi
- Dr Abigail Nyarko Codjoe Derkyi Kwarteng
- Prof Sammy Ohene
- Dr Henry Lawson
- Dr James Akazili
- Ms Linda Lucy Yevoo
- Dr Elizabeth Awini
- Prof Benjamin Uzochukwu
- Dr Annick Tiemele
- Ms Nana Efua Enyimayew
- Ms Grace Aye
- Mr Samuel Ayisi
- Mr Thomas Obeng Anom
- Dr Abraham Hodgson
- Dr Eric Odei
- Dr Leveana Gyimah
- Dr Keziah Naa Amerley Akosua Amarteyfio
- Dr Nyhira Yaw Adjei-Banuah
- Dr Eugene Paa Kofi Bondzie
- Dr Roberta Naa Barkey Ayiku
- Dr Dominic Anaseba
- Mr Labram Massawudu Musah
- Dr Abdul-Basit Abdul-Samed
- Mr Nii Coleman
- Mr Dziedzom Awalime
- Mr Michel Adurayi Amenah
- Mr Cephas Avorka
- Mr Jean Eliel Aye
- Ms Mary Pomaa Agyekum
- Ms Leslie Tetteh Gerbie (Ghana Health Service)
- Ms Abena Boahemaa Amenah
- Mr Wonder Siegward
Website: gcps.edu.gh.
Ashesi University
- Prof Angela Owusu Ansah
- Dr Elena Rosca
- Mr William Ohene Annoh
- Dr Esther Laryea
- Dr Danyuo Yiporo
- Mr David Sampah
- Mr David Sasu
- Mr Ayawoa Dagbovie
- Mr Albert Cofie
- Mr Paul Lamptey
- Mr TsaTsu Agbettor
- Mr Joseph Mensah
Website: www.ashesi.edu.gh.
Laboratoire d'Etudes et de Recherche sur les Dynamiques Sociales et le Développement Local [Research Laboratory on Social Dynamics and Local Development] (LASDEL), Niger
- Prof Aissa Diarra
- Prof Jean Pierre Olivier de Sardan
- Dr Nassirou Ibrahim
- Dr Oumarou Saidou
- Mr Siddo Moumouni
- Ms Aissatou B Sow
- Ms Fatoumata Almahai
- Ms Salamatou Yamba
- Mr, Téoma M. Ousseini
- Mr Farouck Gaoh
- Dr Abdoulaye Ousseini
- Mr Elh. Moustapha Babba Gana Chétima
- Dr Moussa Ismaguel Abdou
- Dr Ousseini Zika Oumou
- Mr Adamou Harouna Hima
- Mr Thierno Diouf
Website: lasdel.net.
Université Catholique de l'Afrique de l'Ouest - Unité Universitaire at Bobo-Dioulasso [Catholic University of West Africa - University Unit at Bobo-Dioulasso] (UCAO-UUB), Burkina Faso
- Dr Maurice Yaogo
- Dr Paolo Ferraris
- Prof Clément Ziemlé Meda
- Dr Ange Nkokolo Massamba
- Dr Vincent-Paul Sanon
- Dr Anicet Touwendsida Kaboré
- Dr Jean Paulin Ki
- Dr Blahima Konaté
- Dr Emilie Pigeao-Gagné
- Dr Jean-André Ki
- Mr Ludovic Deo Gracias Tapsoba
- Mr Yamba Kafando
- Miss Korotime Traoré
- Miss Sana Lisata
- Miss Zagre Cynthia
- Miss Diallo Rasmata
- Mr Simon Konkobo
- Mme Geneviève Ouedraogo
- Miss N’Charick Mafinè Ouattara
- Mr Issoufou Savadogo
- Mr Victor Ouedraogo
- Dr Olivia Marie Angèle Awa Ouedraogo
- Mr Seydou Drabo
- Mr Harouna Padiene
- Mr Sie Ahmed Barro
- Mr Pascal Zoungrana
- Dr Ouedraogo Jean Claude P. Romaric
- Ms Annick Astride Dabire
- Ms Yeli Leticia Yasmine Sou
Website: ucao-uub.com.
Advisory Committee
- Prof. Kerstin Klipstein-Grobusch (Chair) - University Medical Center, Utrecht, The Netherlands. Clinical Epidemiology, NCD. Anglophone
- Dr. Benedict Weobong (Member) - York University School of Global Health, Canada. Researcher. Mental Health. Anglophone
- Prof. Monika Arora (Member) - Executive Director of HRIDAY (Health Related Information Dissemination amongst Youth), Vice President health promotion, Public Health Foundation of India and Chair Global NCD Alliance. Anglophone
- Prof. Roxane Borges Da Silva (Member) - University of Montreal. Public Health /Health Economics. Bilingual
- Prof. Rexford Ahima - John Hopkins University
- Dr. Sylvia Anie (Member) - Independent Consultant. Anglophone
- Prof. Ali Ibrahim Touré (Member) - Université Abdou Moumouni in Niger. cardiology and hypertension management in Africa. Bilingual
- Prof. Kerstin Klipstein-Grobusch
Dr. Kerstin Klipstein-Grobusch, MSc, MSc, PhD, Associate Professor and Head Global Health at the Julius Center for Health Sciences and Primary Care, Department of Global Public Health and Bioethics, University Medical Center Utrecht, The Netherlands & Visiting Professor, School of Public Health, University of the Witwatersrand, South Africa.
Kerstin Klipstein-Grobusch is an epidemiologist and nutrition scientist with over 25 years of experience in international research capacity building and mentoring in epidemiology, public and global health. She is the principal investigator of capacity building training courses and programmes such as CAPSTONE (Capacity Strengthening of Transdisciplinary Education for Non-Communicable Disease Care in West Africa).
She leads the Julius Center’s Global Health research on cardiovascular and cardiometabolic disease related to (i) urbanisation and migration; (ii) double burden of malnutrition; and (iii) communicable and non-communicable co-and multimorbidity. She is the Utrecht based principal investigator on several implementation science projects that aim to improve and scale-up care for hypertension and diabetes in Africa, Asia and Europe such as the iHEART-SA (Integrating heart health in HIV care in South Africa), SCUBY (Scaling-up diabetes and hypertension in vulnerable populations) or MRC-PaLS project (Patient-led support groups in the management of hypertension and diabetes in low-resource settings). She has supervised and mentored over 125 Master, PhD and postdoctoral fellows and published over 300 peer-reviewed papers.
Academic and societal activities include memberships of institutional committees and academic/research networks. Amongst others, she is Editor of the World Health Federations’ scientific journal Global Heart, Chair of the Scientific Advisory Board of the STOP-NCD NIHR Global Health Research Center, and Executive Board Member of the European Global Health Research Institutes Network (EGHRIN).
In her current position as Associate Professor and Head Global Health her focus is on the development of global health research and capacity building (www.globalhealth.eu) at the Julius Center for Health Sciences and Primary Care, University Medical Center Utrecht, The Netherlands.
https://research.umcutrecht.nl/researchers/kerstin-klipstein-grobusch/
- Dr. Benedict Weobong (Member)
-
Associate Professor, York University, Canada
Dr. Benedict Weobong is a global mental health epidemiologist, researcher, and an Associate Professor at the York University School of Global Health, specializing in Mental Health. With a background in psychology and mental health epidemiology from the Universities of Ghana and London, his research is centered on instrument development, perinatal depression, alcohol and substance use, mental healthcare systems, and health promotion interventions.
Dr. Weobong's research portfolio is guided by the principles of global mental health and focuses on four key areas: developing and evaluating psychological treatments, implementation research to scale up evidence-based interventions for mental disorders in primary healthcare, climate change-mental health nexus, and school-based health and wellbeing programs. He utilizes innovative task-sharing strategies to achieve these goals. Currently, his research laboratory is actively developing a step-up care intervention for depression and anxiety among adolescents in Ghana (https://www.kcl.ac.uk/research/african-youth-in-mind), evaluating a routine health check-up program for adolescents, and building a critical mass of global mental health researchers through doctoral and post-doctoral training (https://amari-africa.org).
His impactful research has been funded by prominent organizations including NIHR, GCRF, Fondation Botnar, WHO, FCDO, and the Wellcome Trust. Dr. Weobong serves as an Academic Editor at PloS ONE and is an Editorial Board Member at BMC Psychiatry. Before his tenure at York University, he was instrumental in teaching and supervising students in social and behavioural sciences at the School of Public Health, University of Ghana.
- Prof. Monika Arora (Member)
-
Executive Director, HRIDAY & Vice President (Research), Public Health Foundation of India
Professor Monika Arora is a leading public health scientist specializing in NCD prevention and control and adolescent health. She is the Vice President for Research and Health Promotion at the Public Health Foundation of India (PHFI) and the Executive Director of HRIDAY (Health Related Information Dissemination amongst Youth). Reflecting her global leadership, she is the immediate Past President of the NCD Alliance (2023-25), was the founding Chairperson of the South East Asia NCD Alliance (2020-23), and is a Founding GB member of the Healthy India Alliance.
Professor Arora's research expertise encompasses the design, implementation, and evaluation of Group Randomized Trials, behavioural and mixed-methods research, policy research, implementation research, and the impact evaluation of health policies and programs. Her work has significantly informed National Health Programmes in India and the South East Asia Region. She is an active member of numerous national and international expert committees on NCD Prevention and Control, Tobacco Control, and Ending Childhood Obesity, including the WHO Civil Society Working Group on NCDs. She also served as a Commissioner for the Lancet Commission on Adolescent Health.
Her contributions have been recognized with numerous prestigious awards, including the Best Practices Award in Global Health in 2011 by the Global Health Council, the WHO Director General's World No Tobacco Day Award in 2012, the Exceptional Women of Excellence Award in 2018 by the Women Economic Forum, the Dr. Prem Menon outstanding service award in January 2018 by the World-India Diabetes Foundation (WIDF), and the Society for Adolescent Health and Medicine 2023 International Chapter Award for the Northern Hemisphere.
- Email: [email protected]
- Phone: 91 9810056631
- Online Profile: https://phfi.org/member/prof-monika-arora/
- Twitter: https://twitter.com/DrMonikaArora
- Prof. Roxane Borges Da Silva (Member)
-
Professor and Department Head, University of Montreal, Canada
Professor Roxane Borgès Da Silva is a distinguished academic in the field of public health and health economics. She serves as the Head of the Department (Directrice de département) of Management, Evaluation and Health Policy and is a Full Professor (Professeure titulaire) at the School of Public Health, University of Montreal. Her academic journey includes a Master's degree (Maîtrise) in Econometrics with a specialization in public and health economics from the University of Aix-Marseille II, France (2003), and a PhD in Public Health, specializing in health care organization, from the University of Montreal (2010).
Following her doctorate, she completed a postdoctoral fellowship from 2010 to 2012 in the Department of Epidemiology at McGill University, where she was awarded a 4P program scholarship. Her bilingual expertise lies in the economic evaluation of health policies and the organization of healthcare services.
- Address: École de santé publique - Département de gestion, d'évaluation et de politique de santé, 7101, av. du Parc local 3074-6
- Email: [email protected]
- Phone: 514 343-6031 / 514 985-4000 #4012
- Online Profile: https://espum.umontreal.ca/lespum/departement-de-gestion-devaluation-et-de-politique-de-sante/lequipe-du-departement/personnel-enseignant-regulier/professeur/in/in15778/sg/Roxane%20Borgès%20Da%20Silva/
- Prof. Rexford Ahima (Member)
-
Professor of Medicine, Johns Hopkins University, USA
Professor Rexford Ahima is a globally renowned physician-scientist and a leading authority on endocrinology, diabetes, and metabolism. He is the Director of the Division of Endocrinology, Diabetes, and Metabolism, a Bloomberg Distinguished Professor of Diabetes in the Schools of Medicine, Public Health, and Nursing, and the leader of the Johns Hopkins Diabetes Initiative.
Dr. Ahima's extensive training includes an intercalated BSc in endocrinology from the University of London, an MD from the University of Ghana, and a PhD from Tulane University in 1992. He completed his internal medicine residency at the Albert Einstein College of Medicine and his clinical and research fellowship in Endocrinology, Diabetes, and Metabolism at the Beth Israel Deaconess Medical Center and Harvard Medical School.
His research focuses on the pathogenesis of obesity and diabetes, particularly how circulating factors like adipokines, cytokines, and myokines regulate feeding, glucose, and lipid metabolism. Dr. Ahima is an elected member of the National Academy of Medicine and a fellow of the American Academy of Arts and Sciences, the American Association for the Advancement of Science, the American College of Physicians, and the Obesity Society. He is also a member of the American Society for Clinical Investigation, the Association of American Physicians, and the Interurban Clinical Club. He has held several prestigious editorial roles, including former editor-in-chief of the Journal of Clinical Investigation, former associate editor of Endocrine Reviews, Endocrinology, Molecular Endocrinology, and Gastroenterology, and current editor of the Annals of the New York Academy of Sciences Year in Diabetes and Obesity.
- Email: [email protected]
- Dr. Sylvia Anie CSCI, FRSM, FRSC (Member)
Independent Consultant
Dr. Sylvia Anie is a Chartered Scientist (CSci), a fellow of the Royal Society of Medicine, UK (FRSM), and the Royal Society of Chemistry, UK (FRSC), with a multifaceted career as a scientist, public health and development specialist and an independent consultant. She has extensive experience working internationally and nationally in sectors including education, health, gender, governance, water, sanitation, and hygiene. Her academic background includes studies at the University of Manchester, University College London, and Open University Business School (England).
Dr Anie was selected by the Royal Society of Medicine, UK in March 2022, for a feature on International Day of Women in Science.
Dr Anie worked with the Commonwealth Secretariat, London, as Director for Education, Health and Gender (Social Transformations Programs Division), working across 53 countries and 5 continents. This required enhanced communication, advocacy and networking abilities across countries and the ability to relate to diverse country contexts and priorities.
She represented the Commonwealth Secretariat severally at high level including delivering the statement on Health, Education and Gender Equality at the United Nations General Assembly, New York (2011). During her work at the Commonwealth Secretariat she led in the design of the Commonwealth Gender Policy and engaged in complex international policy making processes and in the crafting of UN declarations working in collaboration with Commonwealth Ambassadors.
In 2015, Dr. Anie was selected to serve on the Board of Trustees for WaterAid UK. She has served on the Boards of the Open Society Foundations, African Research Academies for Women (USA), and served as a Trustee for the Leonard Cheshire Disability Organization in the UK. Dr Anie is also currently a Board Director REVNA Biosciences, a biomedical research facility established to advance molecular diagnosis and facilitate the detection, prevention and treatment of diseases by considering an individual’s genetic makeup.
Her expertise extends to equality, equity, diversity and inclusion. Additionally, Dr. Anie has evidenced experience in youth involvement, mentoring, and coaching. She contributed to the Youth Leaders for Health Programme, a Comic Relief-funded collaboration between WACI Health, RESULTS UK, Hope for Future Generations Ghana, HDT Tanzania, and CISMAT Sierra Leone.
She has been honored for her contributions to scientific knowledge by the Aburi Girls' Senior High School Old Students Association and was recognized as an African Science Hero by the Planet Earth Institute for her research and public health work in improving women's access to health and education.
She has worked as a consulting expert in various countries such as Namibia, South Africa, Kenya, Uganda, Nigeria, Ethiopia, Rwanda, Mauritius, India and Bangladesh and has in depth knowledge of differing country contexts and global developmental challenges.
In her professional life she has and continues to form strategic alliances, initiating and nurturing civil society and private sector engagement. She has worked pro-actively and well with development partners such as UNICEF, UNFPA, World Bank, FAO, FCDO, USAID, WHO etc.
Through her work she has facilitated and driven reforms to protect the marginalized and empower them to demand their health rights and to sharpen access to treatment and care.
- Online Profile: https://ghscientific.com/sylvia-anie/
- Prof. Ali Ibrahim Touré
Ali Ibrahim Touré is a distinguished academic and researcher with a focus on cardiology and hypertension management in Africa. His extensive career includes affiliations with several prominent institutions, such as Université Abdou Moumouni in Niger and Khartoum University in Sudan, where he has contributed significantly to the field of cardiovascular health.
Touré's research is particularly noted for its emphasis on hypertension control and cardiac arrhythmias, addressing critical health challenges faced by populations in Africa. His publications reflect a commitment to improving health outcomes, with notable works featured in respected journals such as the European Heart Journal and The Lancet Global Health. His contributions to the Pan African Society of Cardiology highlight his role in advancing knowledge and practices related to cardiac health across the continent.
In addition to his academic pursuits, Touré has received sponsorship from esteemed organizations, including the National Heart, Lung, and Blood Institute and the Deutscher Akademischer Austauschdienst, underscoring his influence and recognition within the global medical community. His work continues to inspire efforts aimed at enhancing cardiovascular health and addressing the pressing issues of hypertension in Africa.
The Centre’s goal is to contribute to improved health of West African populations through comprehensive and sustainable capacity strengthening for high-quality applied NCD research to improve prevention, diagnosis and management of hypertension, diabetes and related common mental disorders (anxiety, stress, depression). Our ambition is to leave a legacy of person-centred, integrated (not disease-specific) and system-wide (combining staff, structures, resources at multiple levels) responses to inter-connected NCDs at community and primary care levels, through African-led research by high-calibre scholars embedded within supportive institutions, networks and policy environments, all ultimately contributing to reduction in premature mortality from NCDs, improved health, wellbeing and socio-economic benefits.
We will develop generalisable theoretical and practical lessons for effective NCD control and capacity strengthening, through working across diverse language-institutional-socio-economic contexts of Anglophone (Ghana, lower-middle-income) and Francophone (Niger and Burkina Faso, low-income) countries, identified based on their capacity and research needs, and strong academic/policy/community partnerships.
Our objectives are to:
- Deepen understanding of contextual influences and effective pathways to prevention, diagnosis and management of NCDs in West Africa;
- Co-produce with key stakeholders, contextually-adapted packages of interventions for prevention, diagnosis and management of NCDs at community and primary care levels; and conduct formative process evaluation;
- Implement the intervention package through existing health systems in each country, and evaluate its feasibility, acceptability, clinical effects, equitable reach and cost-effectiveness;
- Comprehensively and sustainably strengthen capacities of researchers, communities and decision-makers, for high-quality applied NCD research and its uptake;
- Ensure effective research communication and uptake into policies and practices of patients, communities, service providers, and national/West African decision-makers;
- Continuously engage with key stakeholders at community, sub-national, national levels within each country and within West Africa;
- Establish and maintain equitable partnerships between the West African and UK applicants, through shared leadership and governance arrangements
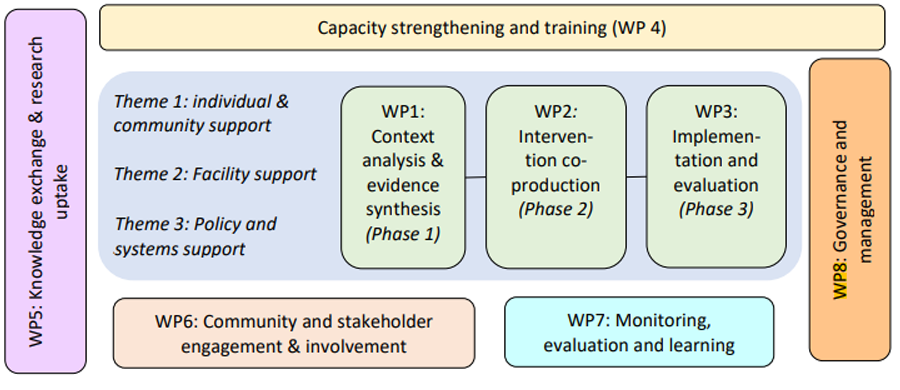
To meet our objectives we will structure activities in eight work packages:
- WP1: Context analysis and evidence synthesis
-
Work package 1 includes: stakeholder analysis and comprehensive analyses of socio-political-cultural-economic contexts of provision and use of NCD services at system, community, household and individual levels, using secondary data analysis, observations and in-depth interviews and a systematic review with a provisional question “which interventions can ensure person-centred, integrated and system-wide responses to inter-connected NCDs in West Africa?”
- WP2: Intervention co-production
-
Work package 2 involves working closely through regular meetings with key stakeholders, including patients, communities, service providers, managers and policymakers, to co-produce context-adapted packages of interventions. We will use our experience in co-production and participatory action research in engaging stakeholders as co-researchers throughout four-step action research cycles, to avoid a ‘travelling model’ approach where effective interventions are carried inappropriately across settings.
- WP3: Implementation and evaluation
-
WP3 focuses on implementation and evaluation of intervention packages. Implementation will be through local structures and processes, to ensure sustainability and we will evaluate feasibility, acceptability, clinical effects, equitable reach, and cost-effectiveness of the interventions packages.
Evaluation of the intervention packages will comprise: formative, using observations, interviews, analysis of service data and documentary analyses; seeking to refine the co-produced intervention packages, and summative quasi-experimental stepped wedge study design, combining analyses of routine service data, periodic household surveys, interviews, focus groups, observations and document reviews.
- WP4: Capacity strengthening and training
-
Work package 4 will target individual, organisational and system-level capacities of researchers, particularly earlier-career staff, and their organisations, for high-quality applied NCD research; communities, to engage and improve behaviours and decisions affecting their health and policymakers and practitioners, to implement evidence-based NCD interventions.
- WP5: Community and stakeholder engagement and involvement
-
Work package 5 will see engagement with communities and stakeholders through regular meetings for co-producing, implementing and evaluating interventions and research uptake. We will establish country-specific multi-stakeholder forums informed by stakeholder analysis to extensively consult with, and ensure representation of neglected community voices in NCD research.
- WP6: Knowledge exchange and research uptake
-
Work package 6 will see the development and implementation of a knowledge exchange and research uptake strategy. This strategy will inform mapping of knowledge preferences and expectations by different stakeholders including communities, practitioners, policymakers as part of the initial analyses and capacity assessments.
- WP7: Monitoring, evaluation and learning
-
Work package 7 will see the development and implementation of a comprehensive monitoring evaluation and learning strategy capturing key milestones to reflect the three research phases. We will use metrics for equitable partnerships, research, capacity strengthening and overall impact in our approach to knowledge exchange.
- WP8 Governance and management
-
Work Package 8 will ensure excellent coordination of the centre, through the development of appropriate, and equitable governance and management arrangements to support the aims of the centre are met and to support continuous communication with the partners and the funder and other key stakeholders.
Our three research themes reflect the level of support for person-centred, integrated and system-wide responses to interconnected NCDs through:
- Individual and community support
- Primary healthcare facility support
- Systems and policy support
Research themes are interrelated, build on, and complement, each other. For example, individual awareness about the nature and importance of NCD risk factors affects health seeking behaviours. Facility-based care is contingent on support for staff and an enabling policy environment.
Work within each theme is organized according to our three research workpackages: context analysis and evidence synthesis intervention co-production and implementation and evaluation Each theme has research questions, to be addressed through country-specific research projects, which will organise resources for generation of evidence.
Our goal is to contribute to improved health and wellbeing of populations in West Africa, through comprehensive and sustainable capacity strengthening for high-quality applied NCD research to inform improved prevention, screening, primary care diagnosis and management/referrals of interrelated hypertension, diabetes and common mental health problems. Our ambition is to leave a legacy of excellent African-led NCD research by high-calibre researchers embedded within supportive institutions and networks, which will contribute to improved health outcomes, wellbeing and wider socio-cultural-economic benefits in West Africa.
Our approach to community engagement and involvement is underpinned by a commitment to transformative engagements with individuals and groups throughout mutually-respectful, inclusive and ethical research. Transformation can take place when the knowledge and experiences of marginalised populations are articulated, understood, and centred within the research; when knowledge-based power is redistributed and mutual learning is centred. We will ensure these through participatory co-production using action-reflection cycles. This will allow our in-depth understanding of the intersecting experiences of marginalisation and exclusion, and enable communities to identify and articulate their needs for information to solve what they perceive as key issues in addressing the inter-related NCDs. The local communities are diverse, and we will be attentive to the power dynamics of these groups.
In each country, we will establish an in-country multi-stakeholder forums comprising 15-20 decision-makers, health workers, managers and practitioners, and civil society organisations. These advisory bodies will also help represent all voices in NCD research and provide platform for cross-stakeholder exchange, engagement, advocacy and joint decision-making.
Central to our plans is engaging and involving people living with NCDs, their families and carers, including those often marginalized. We will support, train and strengthen capacity of people living with NCDs to get involved in the NCD research and control. This will be done through close partnerships with, and supporting the work of, all above-mentioned CSOs working in their respective languages and within relevant social contexts. The rationale for this approach is to build on and extend existing processes and networks rather than create new, and potentially less sustainable, channels.
Our CEI activities will directly shape research to ensure its impact. We will particularly identify, and adapt where feasible, creative approaches to CEI such as photovoice, participatory film-making, local theatres. The continued cross-country peer-exchange, support and sharing will enable mutual learning and maximising impact for the benefit of the local people and communities.
Our goal is to contribute to improved health and wellbeing of populations in West Africa, through comprehensive and sustainable capacity strengthening for high-quality applied NCD research to inform improved prevention, screening, primary care diagnosis and management/referrals of interrelated hypertension, diabetes and common mental health problems. Our ambition is to leave a legacy of excellent African-led NCD research by high-calibre researchers embedded within supportive
institutions and networks, which will contribute to improved health outcomes, wellbeing and wider socio-cultural-economic benefits in West Africa.
We will use comprehensive and sustainable approaches to capacity strengthening, improving individual, organisational and system-level capacities of:
(a) researchers, particularly earlier-career staff, for high-quality applied NCD research,
(b) local communities, to engage with and improve behaviours and decisions affecting their health and
(c) policymakers and practitioners, to implement evidence-based NCD interventions.
This will be achieved through a combination of post-graduate training, short courses and workshops, structured mentorship support, cross-organisational exchange and learning, communities of practice and the co-production process itself.
Current students
The Stop-NCD consortium is currently supporting the following doctorate students:
- Annick Gladzah – conducting a DrPH degree at the London School of Hygiene and Tropical Medicine (2023-present)
- Chephas Ke-on Avoka - conducting a DrPH degree at the London School of Hygiene and Tropical Medicine (2024-present)
- Michel Adurayi Amenah - conducting a PhD degree at Lancaster University (2024-present)
- Mary Atta Pomaa Agyekum - conducting a PhD degree at UMC Utrecht (2025-present)
- Basit Abdul-Basit - conducting a DrPH degree at the London School of Hygiene and Tropical Medicine (2025-present)
- David Sasu
- Abdoul Karim Yamba Salamatou - conducting a PhD degree at Université de Montréal (2023-present)
- Téoma M. Ousseini - conducting a PhD degree (2023-present)
- Elh Moustapha Chétima - conducting a PhD degree (2023-present)
- Dr Vincent Paul Sanon
- Trarore Isskandariatou Korotime - conducting a PhD degree at Université Nazi Boni (UNB) (2023-2026)
- Zagre P. Cynthia Severine – conducting a Master’s degree at UCAO-UUB (2023-2026)
- Sana Lisata – conducting a Master’s degree at UCAO-UUB (2023-2026)
- Diallo Rasmata – conducting a Master’s degree at UCAO-UUB (2022-2025)
- Tapsoba ludovic deo gracias – conducting a PhD at the Université Joseph KI Zerbo (2023-2026)
Graduates
We are pleased to congratulate members of the Stop-NCD teams:
Ellen B. Peprah graduated from Johns Hopkins School of Public Health & Carey Business School. She obtained Master of Public Health (MPH) and Master of Business Administration (MBA).
Ama Akoma Essuman graduated from Johns Hopkins School of Public Health & Carey Business School. She obtained Master of Public Health(MPH), Master of Business Administration(MBA), and a certificate in Quality, Patient Safety, and Outcomes Research.
The NIHR Global Health Research Centre for non-communicable diseases in West Africa is part of the NIHR and hosted by LSHTM and GCPS.
We are committed to embedding our work in the contexts we are working in though working closely with stakeholders at all levels of the heath and research systems.
Articles in peer-reviewed journals
Disparities in the access and provision of mental health services as part of primary health care: a case study of Ga-South district in the Greater Accra region
Abena Boahemaa Adusei, Roberta Naa Barkey Ayiku, Kezia Akosua Naa Amerley Amarteyfio, Nhyira Yaw Adjei-Banuah, Abdul-Basit Abdul-Samed, Tolib Mirzoev, Irene Akua Agyepong (2025) Frontiers in Public Health | https://doi.org/10.3389/fpubh.2025.1537955
Effectiveness of lifestyle interventions for glycaemic control among adults with type 2 diabetes in West Africa: a systematic review and meta-analysis protocol | Systematic Reviews
Ellen Barnie Peprah, Yasmin Jahan, Anthony Danso-Appiah, Abdul-Basit Abdul-Samed, Tolib Mirzoev, Edward Antwi, Dina Balabanova, Irene Agyepong (2024) SpringerNATURE | https://doi.org/10.1186/s13643-024-02555-8
Estimating the prevalence, socioeconomic determinants, and health seeking behavior of individuals with depression in Ghana | Scientific Reports
Michel Adurayi Amenah, Ama Fenny, James Akazili, Tolib Mirzoev, Irene Akua Agyepong & Thomas Mason (2025) National LIbrary of Medicine | PMID: 40596148 | PMCID: PMC12215751 | https://doi.org/10.1038/s41598-025-06134-2
Exploring the path to optimal diabetes care by unravelling the contextual factors affecting access, utilisation, and quality of primary health care in West Africa: A scoping review protocol | PLOS One
Abdul-Basit Abdul-Samed, Ellen Barnie Peprah, Yasmin Jahan, Veronika Reichenberger, Dina Balabanova, Tolib Mirzoev, Henry Lawson, Eric Odei, Edward Antwi, Irene Agyepong (2024) PLOS One | https://doi.org/10.1371/journal.pone.0294917
Factors influencing primary care management for patients living with hypertension in West Africa- A scoping review protocol
Kezia Naa Amerley Akosua Amarteyfio, Eugene Paa Kofi Bondzie, Veronika Reichenberger, Irene Akua Agyepong, Evelyn K Ansah, Aissa Diarra, Tolib Mirzoev, Pablo Perel, Maurice Yaogo, Edward Antwi (2024) BMJ Open | doi: 10.1136/bmjopen-2023-077459
Factors influencing access, quality, and utilization of primary health care for patients living with hypertension in West Africa - A scoping review
Kezia Naa Amerley Akosua Amarteyfio, Eugene Paa Kofi Bondzie, Veronika Reichenberger, Nana Efua Enyimayew Afun, Albert Kofi Mensah Cofie, Mary Pomaa Agyekum, Paul Lamptey, Evelyn K Ansah, Irene Akua Agyepong, Tolib Mirzoev, Pablo Perel (2024) BMJ Open | https://doi.org/10.1136/bmjopen-2024-088718
Factors influencing primary care access for common mental health conditions among adults in West Africa: protocol for a scoping review
Nhyira Yaw Adjei-Banuah, Veronika Reichenberger, Roberta Naa Barkey Ayiku, Eugene Paa Kofi Bondzie, Kezia Naa Amerley Akosua Amarteyfio, Mary Pomaa Agyekum, Tolib Mirzoev, Adrianna Murphy, Sammy Ohene, Edward Antwi, Irene A. Agyepong (2024) JMIR Publications | https://www.researchprotocols.org/2024/1/e58890 | DOI: 10.2196/58890
Impact of health systems interventions in primary health settings on type 2 diabetes care and health outcomes among adults in West Africa: A systematic review protocol
Eugene Paa Kofi Bondzie, Kezia Amarteyfio, Yasmin Jahan, Dina Balabanova, Tony Danso-Appiah, Tolib Mirzoev, Edward Antwi, Irene Agyepong (2024) PLOS One
Impact of health systems interventions in primary health settings on type 2 diabetes care and health outcomes among adults in West Africa: A systematic review
Eugene Paa Kofi Bondzie, Kezia Amarteyfio, Yasmin Jahan, Nana Efua Enyimayew Afun, Mary Pomaa Agyekum, Ludovic Tapsoba, Dina Balabanova, Tolib Mirzoev, Irene Agyepong (2025) PLOS One | https://doi.org/10.1371/journal.pone.0319478
Incidence, prevalence and risk factors for comorbid mental illness among people with hypertension and type 2 diabetes in West Africa: protocol for a systematic review and meta-analysis
Roberta Naa Barkey Ayiku, Yasmin Jahan, Nhyira Yaw Adjei-Banuah, Edward Antwi, Elizabeth Awini, Sammy Ohene, Irene Akua Agyepong, Tolib Mirzoev, Mary Amoakoh-Coleman (2024) BMJ Open | PMID: 39609030 | doi:10.1136/bmjopen-2023-081824
STOP-NCD Newsletter
STOP NCD in the news
- Deuxième atelier de coproduction des interventions du programme NIHR-STOP-NCD
- Atelier de coproduction des interventions du Programme Stop-Maladies Non Transmissibles au Niger: Aligner les efforts pour rendre les interventions plus efficaces
- Dosso/Santé: Deuxiime atelier de co- production des interventions du programme action Stop-NCD
- There is poor funding for the NCD prevention and control programme-Research
- Let’s use telemedicine to improve medical care in rural communities – Prof. Agyepong
- GCPS, partners launch Stop-NCD campaign to strengthen healthcare systems
- There is poor funding for the NCD prevention and control programme-Research
- Non-Communicable Diseases (NCDs) awareness and understanding lacking — Prof Agyepong
- There is poor funding for the NCD prevention and control programme-Research
- There is poor funding for the NCD prevention, control programme — Research Team
- Let’s use telemedicine to improve medical care in rural communities – Prof. Agyepong
- Ghana must do more to raise awareness on Non-Communicable Diseases – Prof Agyepong
- GCPS, partners launch Stop-NCD campaign to strengthen healthcare systems
- Non-communicable diseases awareness and understanding lacking – Prof Agyepong