Over the past 15 years, malaria infections have halved across Africa, yet in 2013 more than 3 billion people remained at risk of the disease globally. This year, the first vaccine against malaria – RTS,S – completed clinical trials and showed some level of protection, but will it be enough?
Meera Senthilingam investigates where a vaccine will fit into the current fight against malaria and explores what’s left to tackle the disease once and for all.
The buzz comes abruptly. A squealing buzz causing sensations across the surface of the skin, bringing with it anticipation of blood being drawn and skin being raised. For some, this buzz is merely a symbol of summertime, or warmer climates, or a mother trying to feed her young. But in 97 countries across the globe, this familiar sound strikes a nerve, many nerves. Here, this sound of a tiny mosquito hovering nearby hits nerves beyond the senses of sound or touch — it invokes fear.
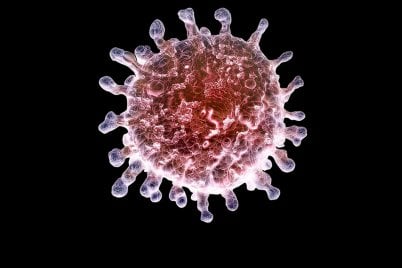
These 97 countries and territories are endemic for malaria, a blood-borne parasitic infection spread only by the bite of a female Anopheles mosquito and killing almost 500,000 people each year. The saliva, not the bite, is what they truly fear. It’s the saliva from these female mosquitoes, which is filled with thousands of microscopic parasites, ready to infest any human within their reach. “One of these parasites alone could kill you,” says Sir Brian Greenwood, Professor of Clinical Tropical Medicine at the London School of Hygiene and Tropical Medicine, referring to the multiple parasites primed and waiting to invade the human bloodstream.With thousands lurking in the saliva, approximately ten injected in each bite, and just one plasmodium parasite needed to cause disease, the risk of infection is high.
An estimated 3.3 billion people are at risk of malaria, according to the World Health Organization (WHO), and 90% of them are in Africa. “Malaria is a very difficult disease to deal with,” says Prof Greenwood. Plasmodia have a complicated life cycle traversing both human and mosquito hosts and passing through varying reproductive stages within each host. In humans, just a few minutes is enough for parasites to get from the site of a bite, through the blood and into the liver. This is where the real damage begins.
“The parasite is quite vulnerable at that stage,” says Prof Greenwood making this point in time the perfect opportunity to stop the infection in its tracks — before thousands, and then billions, of parasites take over the blood. Over the past 30 years, hope has been emerging slowly with a potential vaccine on the horizon targeting this exact stage of infection – the RTS,S vaccine.
The complexity of a simple vaccine
“Having a vaccine to control an infectious disease is the simplest, and probably the cheapest way [to control it],” says Prof Greenwood. But having a vaccine against malaria has been a challenge from the outset, due in large part to the parasite’s complex biology. Its genetic structure, numerous stages of development and ability to avoid immune attack make it a slippery villain to track down – and keep down.
“You can knock out one bit of it with a vaccine…and it has ways of getting around that problem,” says Prof Greenwood who has played a role in the development of RTS,S. This undefeated survival of the parasite is showcased by the fact that adults exposed to, and infected with, malaria on numerous occasions continue to be susceptible to further infections. “Now we are trying to do even better… with an artificial vaccine,” explains Prof Greenwood.
The RTS,S phase three vaccine trial was the largest of its kind to date, working with more than 15,000 children across 11 trial sites in 7 sub-Saharan African countries, spanning populations representing the true burden of malaria. One key part of the design was the testing of two different age groups of children – one aged 5-17 months, and the other aged 6-12 weeks. The earlier the protection, the greater the number of lives that could be saved and the easier it would be to administer the vaccine as part of routine vaccination schedules. The results are now in, but have many questions in tow.
In the study published in the Lancet in April 2015, the RTS,S vaccine was shown to provide 36.6% protection over a period of nearly four years in the older age-group of children when given as three monthly doses of the vaccine along with a booster one year later. The protection in infants was lower, with just 25.9% efficacy when given the same doses. An additional limitation was that protection waned over 12-18 months without a booster dose.
“So we have a vaccine that gives you some, but not terribly good, protection and it wanes quite quickly,” says Prof Greenwood. The questions now arising for all those in the control community are: Do we use it? And if so, how do we use it most effectively?” The European Medicines Agency (EMA) has given a positive opinion on the findings and the world now awaits WHO guidelines to be set to gauge the reality of implementation in the field. “Whilst we are happy with these results, the entire public health relevance of this remains to be determined,” says Dr Pedro Alonso, Director of the WHO Global Malaria Programme.
The organization’s advisory committee on malaria will soon determine this relevance. However, one fact both WHO and scientists at the School agree upon is that this is not the end of the road for malaria vaccines — a higher level of protection is needed. “Clearly this is not a definitive vaccine and should act as an incentive for further research and development,” says Dr Alonso. Stronger protection is needed for a true game-changer to emerge triumphant. “The type of vaccine we will be needing with 80 or 90% protection is still not in our hands,” Dr Alonso says. The somewhat lower than expected results have, however, brought hope that better vaccines are possible.
More importantly, the trial itself has set a precedent for how vaccines should be tested and has trained local scientists the skills needed to design and conduct vaccine trials in the future. But the nature of the parasite means a game-changer may never be on the cards. “We’re not going to have a malaria vaccine that gives 100% protection for many years,” says Prof Greenwood. If that is the case, what’s next?
Fitting a vaccine into the master plan
“If you went to a malaria control program manager and offered them the chance for 30-40% less malaria cases, they would say yes,” says Professor Chris Drakeley, Director of the Malaria Centre at the London School of Hygiene & Tropical Medicine. Prof Drakeley, like most in the malaria research community, believes the vaccine has a role to play in countries with the highest burden of malaria. “You can see a benefit in reducing 30% of cases in those high transmission settings,” he adds. As it stands, the vaccine is likely to be an intervention used alongside those already in use, which to date have made a large dent in numbers of malaria cases globally.
This was exemplified in the phase three trial with all children given insecticide-treated nets to sleep underneath. The impact of current interventions has been particularly notable in Africa where the majority of the burden, and cases of severe malaria, occur. According to a recent report published in Nature, the overall number of malaria infections on the African continent have halved since the year 2000, and more than 660 million infections have been prevented by current control interventions.
Key interventions to date have been improved diagnostic tests, improved drug treatment, and large-scale distribution of insecticide treated bed nets. “This deployment in the last 15 years has resulted in unprecedented gains,” says Dr Alonso.The greatest impact identified in the Nature report was with insecticide-treated nets, reported to have been responsible for 68% of the cases prevented. “[Nets] have had the largest impact essentially because they are a prevention tool,” says Dr Alonso.This aligns with the key public health principle that prevention is better than cure.
However, tests and treatments have also played their part, proving they are essential in helping reduce the number of severe infections and deaths. “All those have combined to see the global reductions in malaria transmission we’ve seen,” says Prof Drakeley. But right now, there’s no time for complacency. Despite these reductions in numbers, there were still almost 200 million cases of malaria in 2013 and more than 400,000 deaths mostly among African children. This is due in some part to resistance emerging amongst both parasite and mosquito populations. “We’re noticing the insect vectors are becoming resistant to some insecticides [used] on those nets,” says Prof Drakeley.
What’s more, fuel is being added to the fire by parasites developing resistance against the drugs used to kill them. This is a larger cause for concern in South-East Asia where resistance has already arisen against artemisinin combination therapy (ACT), the current first-line treatment against malaria. Resistance to ACT drugs is yet to arrive on the African continent.
Battling resistance
Teams at the School are pioneering new approaches and interventions to tackle the problems surfacing from current interventions. “We need to make sure we’re ahead of the game,” says Prof Drakeley whose centre is investigating a range of options including new insecticide combinations and means of applying them, new drug treatments including their use as prevention, and improved diagnostic tests with increased sensitivity. The result is hoped to be a new arsenal of weapons to kill both vector and parasite.
In 2013, 53 countries reported resistance among mosquitoes to at least one insecticide used as a means of control. The worry among some in the field when developing insecticide-treated nets is not the insecticides themselves, but instead finding ones that bind well onto the surface of the nets. “We were very lucky with pyrethroids,” says Prof Greenwood about the insecticide currently used on bed nets. These compounds were found to incorporate well into a fibre, he explains, “With a lot of other insecticides that wouldn’t have been possible.”
Other insecticides have instead been used as part of an intervention known as Indoor Residual Spraying (IRS), where insecticides are sprayed onto the walls of homes in high-burden areas. This reduces new infections by killing mosquitoes as they rest on the walls of a home. The strategy was once highly effective as a means of reducing new malaria infections, but its increased cost and difficulty to deliver in the field has led to IRS being used less frequently today. “Getting these insecticides into a second generation of nets is a priority,” says Prof Greenwood.
Teams at the Malaria centre are collaborating with insecticide manufacturers and other research groups working on this locally to both develop new insecticides as well as reinvigorate existing ones to make them more persistent when applied to nets. “It’s evaluating new compounds but also optimally using existing ones,” says Prof Drakeley. This same rule applies to tackling drug resistance, which Prof Drakeley has equal concerns about. “We cannot have the cupboard bare in terms of alternative drugs,” he says. If resistance reaches Africa, as happened with past antimalarial chloroquine, the result would have severe consequences. “Chloroquine resistance in the early 90’s [saw] mortality for malaria increase massively,” says Prof Drakeley. Teams are therefore currently trying to fill the cupboard with alternatives in order to avoid this devastating scenario occurring again.
T’is the season
Old antimalarial drugs are also being harnessed to help pioneer one key intervention being spearheaded by the School – known as seasonal chemoprevention. This recently adopted strategy protects children living in highly endemic, but seasonal, regions of Africa where malaria transmission occurs during just a few months each year. The goal is to provide long-lasting antimalarials ahead of a surge in new infections to act as a shield against parasitic invasion. But crucially, the use of these drugs must be timely, ahead of known peaks of infection.
“This is a new form of malaria control,” says Dr Paul Milligan, Reader in Epidemiology and Medical Statistics at the London School of Hygiene & Tropical Medicine, who has been trialling the new strategy. The approach involves targeting countries in the sub-Sahel belt of Africa during their rainy season when mosquito numbers – and therefore malaria — are highest. “It’s an example of a different way of thinking about malaria control,” says Dr Milligan.
The slow-release drugs, sulfadoxine-pyrimethamine and amodiaquine, are taken once a month by children during their country’s rainy season. Use of these past antimalarials also ensures current ACTs remain available to rapidly treat anyone infected. “These drugs are eliminated from the body slowly and so give a high degree of protection for about four weeks,” says Dr Milligan. Monthly doses are then needed throughout the rainy season to continue protection. A string of trials has provided a large amount of evidence in favour of seasonal chemoprevention, assessing not only the impact of taking drugs seasonally, but the realities of this being implemented and accepted by the communities being targeted.
The adoption of this intervention began with a PhD project, supported by Prof Greenwood and colleagues at the School, testing the strategy in Senegal. The small-scale trial found that giving children under five years a monthly dose of an antimalarial drug for three months reduced the incidence of malaria by 86%. Further studies in Burkina Faso and Mali found the use of chemoprevention to further aid prevention in areas where bed nets were already in use – reducing numbers of uncomplicated malaria infections in children by 77%.
This approach made WHO policy in 2012 after 10 years in development by African scientists in endemic areas supported by the School. “[This] has been shown to very significantly reduce the risk of disease and possibly dying,” says Dr Alonso, who backs the intervention. Seasonal chemoprevention is currently being implemented in eight countries within Africa where populations are now able to keep one step ahead of the rains – and parasites.
Seasonal RTS,S?
The benefits seen in boosting protection within communities ahead of an expected surge of malaria infections is being contemplated as one use for RTS,S. Such an approach would overcome the limitation of the vaccine’s efficacy waning over time as boosters could be given annually. “It might make sense to try to time those boosters just before each transmission season,” says Dr Milligan. The vaccine would provide lower levels of protection than drugs currently used for seasonal chemoprevention, but would remove the need for people to visit health clinics each month to receive their drug supplies. “Where the season is longer it might be attractive to be able to give a single booster dose of vaccine,” says Dr Milligan.
For now, this is simply an idea and trials are needed. “It’s not how you would want to use a vaccine, but given this is what we have that may be one use,” adds Prof Drakeley, who sees the possibility to further curb transmission. Prof Drakeley’s research focuses on malaria transmission, identifying the main hotspots and people responsible for spreading infections within a population, to then be able to target them with relevant interventions. Whilst the world awaits decisions to be made and actions to be put in place regarding RTS,S, the other weapons in the malaria battle need some nurturing.
They need to not only be upgraded, but also to be further utilised in order to reach WHO goals of 90% reduction in disease and death by 2030. “These are not aspirational goals…but are rooted on what can be achieved with currently available tools,” says Dr Alonso. An estimated 50% of the population at-risk in Africa remain unreached by insecticide-treated nets and up to 60 million remain undiagnosed and untreated. But they can – and will –be reached. Some optimism is in the air surrounding these mosquitoes.
Whilst the biggest burden of disease may lie in sub-Saharan Africa, other countries are laying a path for the continent to follow. “In other parts of the world, malaria has been, and continues, to be eliminated,” says Dr Alonso. Argentina is one example that hopes to be certified malaria-free in 2016 and the Euro region of WHO, which includes Central Asia, has had zero cases of malaria this year.
Further still, countries across South-East Asia are now advancing towards elimination.In Dr Alonso’s eyes, the map is shrinking for mosquitoes to harbour this fatal parasite. “Countries are eliminating malaria and we are now contemplating elimination efforts within sub-Saharan Africa,” he says encouragingly. So one day that squealing buzz lurking close to your ear may purely bring mild fears of itchy skin and aesthetic displeasure, but not of death and disease — regardless of where you are in the world.
Cover images courtesy of GSK

![Malaria predominantly affects rural regions of sub-Saharan Africa. [Credit: Paul Milligan/LSHTM] Malaria predominantly affects rural regions of sub-Saharan Africa. [Credit: Paul Milligan/LSHTM]](/sites/default/files/styles/in_page_carousel/public/rural-sub-saharan-africa.jpg?itok=wJmX0_i8)
![A mother receives an insecticide-treated net in the Democratic Republic of Congo. [Credit: LSHTM/Valentina Buj] A mother receives an insecticide-treated net in the Democratic Republic of Congo. [Credit: LSHTM/Valentina Buj]](/sites/default/files/styles/in_page_carousel/public/CMYK%20bednet%20distribution%20-%20E%20C.jpg?itok=AufwXnPK)
![A community health worker shows a grandmother how to put up a bed net. [Credit: GSK] A community health worker shows a grandmother how to put up a bed net. [Credit: GSK]](/sites/default/files/styles/in_page_carousel/public/health-worker-fixes-bednet-crop.jpg?itok=boGGVhBj)
![Insecticide residual spraying (IRS) involves walls of homes being sprayed with insecticides to kill mosquitoes as they rest. [Credit: Jess Critchley/LSHTM] Insecticide residual spraying (IRS) involves walls of homes being sprayed with insecticides to kill mosquitoes as they rest. [Credit: Jess Critchley/LSHTM]](/sites/default/files/styles/in_page_carousel/public/insecticide-sprayed-Jess-Critchley.jpg?itok=-osicioN)
![Blood samples are needed for diagnosis of malaria. [Credit: GSK] Blood samples are needed for diagnosis of malaria. [Credit: GSK]](/sites/default/files/styles/in_page_carousel/public/blood-sample-malaria-testing.jpg?itok=JL1nBdI8)
![Rapid diagnostic tests have improved detection of malaria cases in the field. [Credit: Paul Milligan/LSHTM] Rapid diagnostic tests have improved detection of malaria cases in the field. [Credit: Paul Milligan/LSHTM]](/sites/default/files/styles/in_page_carousel/public/rapid-diagnostic-tests.jpg?itok=sMX59SRi)
![More accurate diagnosis is enabled through analysis of blood samples in the lab. [Credit: GSK] More accurate diagnosis is enabled through analysis of blood samples in the lab. [Credit: GSK]](/sites/default/files/styles/in_page_carousel/public/microscope-blood-sample.jpg?itok=2pekh6Ub)
![The main treatment for malaria is artemisinin combination therapy (ACT). [Credit: Arturo Sanabria/Photoshare] The main treatment for malaria is artemisinin combination therapy (ACT). [Credit: Arturo Sanabria/Photoshare]](/sites/default/files/styles/in_page_carousel/public/malaria-act-treatment.jpg?itok=S_h6zKP0)
![Warehouse workers package ACTs with Rapid Diagnostic Tests (RDTs) in Mozambique. [Credit: Arturo Sanabria/Photoshare] Warehouse workers package ACTs with Rapid Diagnostic Tests (RDTs) in Mozambique. [Credit: Arturo Sanabria/Photoshare]](/sites/default/files/styles/in_page_carousel/public/warehouse-in-mozambique-package-acts-and-rdts.jpg?itok=dDf_iPwW)
![Community health teams deliver seasonal chemoprevention in Senegal. [Credit: Paul Milligan/LSHTM] Community health teams deliver seasonal chemoprevention in Senegal. [Credit: Paul Milligan/LSHTM]](/sites/default/files/styles/in_page_carousel/public/community-health-teams-senegal.jpg?itok=hpgeUXYo)
![A child receives seasonal chemoprevention with long-lasting antimalarial drugs. [Credit: Paul Milligan/LSHTM] A child receives seasonal chemoprevention with long-lasting antimalarial drugs. [Credit: Paul Milligan/LSHTM]](/sites/default/files/styles/in_page_carousel/public/child-receives-antimalarial-drugs_Paul-Milligan.jpg?itok=biQ7ONHP)
![Community healthworkers deliver chemoprevention services to rural villages in Senegal. [Credit: Paul Milligan/LSHTM] Community healthworkers deliver chemoprevention services to rural villages in Senegal. [Credit: Paul Milligan/LSHTM]](/sites/default/files/styles/in_page_carousel/public/community-health-workers-deliver-senegal.jpg?itok=Pz8b_dYi)