Stronger-SAFE is a five-year project that will increase our understanding of how trachoma is transmitted, leading to the development and testing of new, more effective interventions and treatment approaches. We are funded by the Wellcome Trust through a Collaborative Award.
We are an interdisciplinary team from the London School of Hygiene & Tropical Medicine, Ethiopian Ministry of Health, The Fred Hollows Foundation, the Wellcome Trust Sanger Institute and Monash University.
200 million people still live in trachoma-endemic regions and are at risk of becoming blind despite concerted international effort to tackle the disease. With the clock ticking towards the 2020 elimination goal, novel strategies are urgently needed to accelerate and strengthen the SAFE strategy.
What is Stronger-SAFE?
Stronger-SAFE is a Wellcome Trust funded project that will increase our understanding of how trachoma is transmitted, and hopefully lead to the development and testing of new, more effective interventions and treatment approaches. The five year study is based in Ethiopia where the disease is highly endemic, with partners the Ethiopian Ministry of Health, the Oromia Regional Health Bureau, The Fred Hollows Foundation, the Wellcome Trust Sanger Institute and Monash University in Australia.
Trachoma in Ethiopia
Trachoma is an eye disease caused by infection with the bacterium Chlamydia trachomatis. Around 190 million people worldwide live in endemic areas and require treatment. Trachoma is thought to spread through person-to-person contact and by flies that have been in contact with discharge from the eyes of an infected person. The disease is responsible for 3% of the world's blindness, with more than 80% of the burden of active trachoma concentrated in 14 Sub-Saharan African countries. Ethiopia is the most severely affected country.
The World Health Organization Alliance for the Global Elimination of Trachoma by 2020 (GET2020) recommends the SAFE Strategy: Surgery for trichiasis, mass distribution of the antibiotic Azithromycin to treat chlamydial infection, Facial cleanliness and Environmental improvement to suppress transmission.
Stronger-SAFE involves three phases:
- Phase 1: Studying transmission in trachoma
- Phase 2: Understanding and changing behaviour
- Phase 3: Testing Novel Approaches to strengthen ‘A’ and ‘F&E’ in SAFE (Stronger-SAFE)
Bart Versteeg
Adam Biran
Oumer Shafi
PhD student

Ailie Robinson
Research Fellow
Collaborators
Biruck Kebede Negash, Director of Disease Prevention & Control Directorate, Federal Ministry of Health, (Ethiopia)
Fantahun Tadesse, (Ethiopia)
Nazif Jemal, Communications Coordinator, The Fred Hollows Foundation (Ethiopia)
Nicholas Thomson, Group Head, Infection Genomics Program, Wellcome Trust Sanger Institute (UK)
Manoj Gambhir, Associate Professor, Monash University (Australia)
Sarity Dodson, Global Lead, The Fred Hollows Foundation (Australia)
Virginia Sarah, Global Partnership Executive, The Fred Hollows Foundation (UK)
Yeneneh Mulugeta Deneke, Country Director, The Fred Hollows Foundation (Ethiopia)
Zelalem Jemal, The Fred Hollows Foundation (Ethiopia)
Lab Manager, Oromia Regional Health Board, Ethiopia
In order to allow participants in the Stronger SAFE project to give feedback about their experiences and share our activities more widely, we created some videos with participants featuring their views on taking part in the project.
Our first video will be shown in different areas of Ethiopia (originally in areas not currently part of the trial) to share the project and the benefits of taking part in research:
Our second video gives an overview of Stronger SAFE and its aims, featuring one of the project’s researchers:
This is a reproduction of the post originally published on http://iceh.lshtm.ac.uk here.
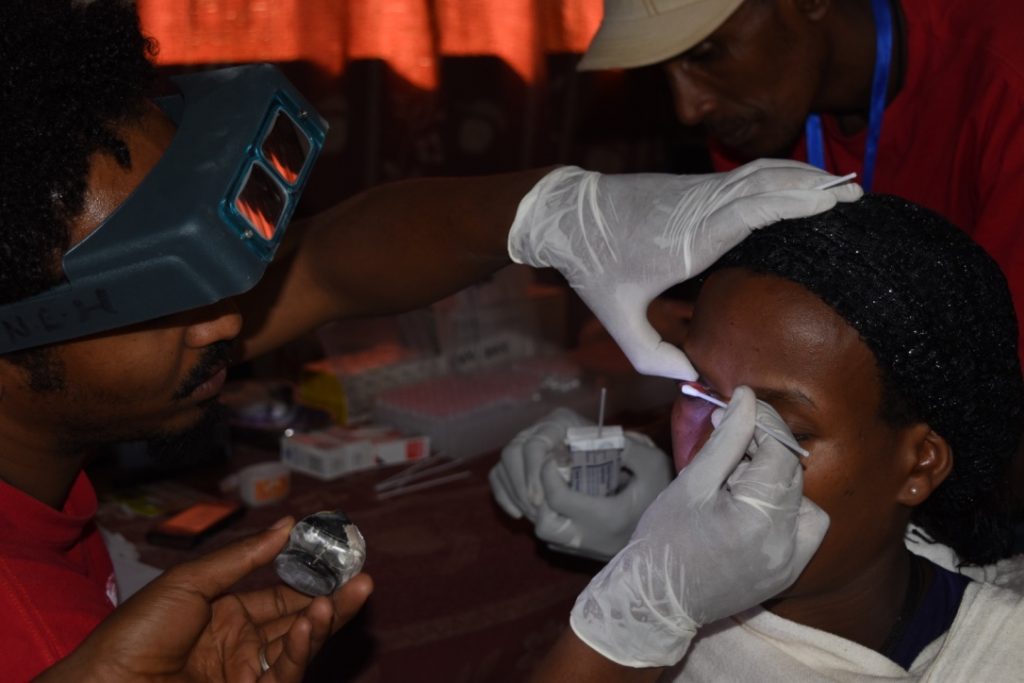
 Esmael Habtamu Ali with patient during Trachoma field work in Ethiopia
Esmael Habtamu Ali with patient during Trachoma field work in Ethiopia
Register for the Eliminating Trachoma course here: https://www.futurelearn.com/courses/eliminating-trachoma/5
Esmael Habtamu Ali PhD, Co-Lead Educator
Why Trachoma?
My country, Ethiopia, has amongst the highest levels of avoidable blindness in the world. Cataract, corneal opacities from trachoma and refractive error are the leading causes of blindness.1 Trachoma is one of the most common Neglected tropical Diseases, and the leading infectious cause of blindness worldwide affecting the poorest of the poor.2,3 It is prevalent in developing and marginalised communities, particularly in Africa, where crowded living conditions are common and access to clean water, sanitation and health care are often limited.4-6
The blindness in trachoma is the result of the painful trachomatous trichiasis (eye lashes scratching the surface of the eye) due to enrolling of the eyelids (entropion) caused by conjunctival scarring provoked by the chronic inflammation and infection from the bacteria Chlamydia trachomatis. Trachomatous Trichiasis (TT) causes considerable pain leading to functional and physical impairment, social withdrawal and exclusion, and inability to work and earn an income even prior to the development of visual impairment.7,8
Trachoma can be easily prevented and treated. The WHO Alliance for the Global Elimination of Blinding Trachoma by 2020 (GET2020) recommends the SAFE Strategy to control trachoma.9 This involves Surgery to avert the risk of blindness from trachomatous trichiasis, together with Antibiotics (azithromycin or tetracycline), Facial cleanliness and Environmental improvements to suppress chlamydial infection and transmission. However, despite the extensive global effort trachoma is still a public health problem in 42 countries.2
Currently, about 200 million people live in trachoma endemic areas.2 Approximately 3.2 million people have un-treated TT and are at significant risk of sight loss, and 2.4 million people are visually impaired from trachoma of whom 1.2 million are irreversibly blind.2Africa is the most affected continent from trachoma. About 18.3 million cases with infection and 2.24 million TT cases are found in Africa.10 This accounts for 85.3% and 70.9% of the active trachoma infection and TT cases worldwide. Three African countries (Ethiopia, Malawi and Nigeria) account for 50% of the trachoma at risk population worldwide. Four African countries (Ethiopia, Nigeria, Egypt and Uganda) account for more than 43% of the global TT surgical backlog.2
Ethiopia carries the largest burden of trachoma worldwide. About 75 million people are at risk of infection, more than 138,000 are irreversibly blind, and another 700,000 are at immediate risk of painful irreversible blindness from trachoma.2 Perhaps more than any other country in the world, in Ethiopia, enormous amount of effort is required to eliminate blinding trachoma. The millions of people who are at risk of blindness from trachoma need immediate surgery to correct the TT. It is this unnecessary suffering of communities inspired me to join the global task force to eliminating trachoma as a public health problem.
Professional Background
I completed the undergraduate ophthalmic officer course with Great Distinction at the University of Gondar in 2007. Between 2007 and 2010, successfully coordinated large collaborative research project on the management of the blinding stage of trachoma. In 2011 I won scholarship for MSc in Community Eye Health at LSHTM, UK and won the Gordon Johnson Prize for outstanding performance. I used this chance to grasp the appropriate skill and knowledge that I require to run effective eye care research projects and programmes in Ethiopia. After completing the MSc course at the LSHTM, I was involved in a project documenting “best Practices” in Zithromax Mass Drug Administration (MDA) (a drug distributed to control the pool of trachoma infection in communities). I visited six different trachoma control programmes in Ethiopia, Nigeria and Kenya and wrote case studies on Zithromax MDA from which best practices have been extracted and compiled in to a manual to guide trachoma control programmes.11
In In 2017 I completed my PhD on the surgical management of trachomatous trichiasis and it’s impact on quality of life. I was awarded the 2017 LSHTM Woodruff Medal for the outstanding doctoral thesis completed that year. In my PhD project, we provided community based surgical management to more than 2500 people suffering from the blinding stage of trachoma, in Ethiopia. We trained more than 400 community members from the health development army to screen, identify and refer trachoma cases that need surgical management. In this project, we compared two commonly used surgical procedures in randomised controlled trial (bilamellar tarsal rotation (BLTR) and posterior lamellar tarsal rotation (PLTR). We found that the PLTR is superior to the BLTR with lower rate of recurrence and complications.12 The results led to a shift in policy and currently WHO recommends that new surgical trainees in programs should be trained in the PLTR procedure.13
The Final Push to Eliminate Trachoma
The WHO led Global Alliance for the Elimination of Trachoma by 2020 (GET2020) is a couple of years away. Given the huge backlog, Ethiopia should make extra efforts to achieve this goal. For instance, with regard to averting the risk of blindness, in Ethiopia, we are facing two different challenge: There are still communities losing their eyesight from severe trachomatous trichiasis as they do not have access to surgical services; while on the other hand there are communities with access to surgical services but hesitant to utilise the service in relation to awareness and the quality of service being provided. We have previously demonstrated that training and deploying community members for the identification, counselling and referral of TT cases in their community could be the most productive approach to increase uptake of TT surgery. Much more need to be done on the F and E components of the SAFE strategy to break trachoma infection transmission through enhanced community involvement and ownership.
Building Capacities
The free online course, Eliminating Trachoma, is designed to build the capacities of district and community level trachoma control program implementers and mangers around the world involved in a fight to eliminate trachoma as a public health problem. It will help to identify the challenges that we are facing in the final few kilometres in the race to beating trachoma by 2020. It will provide an opportunity to discuss solutions and get insights from various experts in the field to address the gaps in own setting.
Register for the Eliminating Trachoma course here: https://www.futurelearn.com/courses/eliminating-trachoma/5
- Berhane Y, Worku A, Bejiga A. National survey on blindness, low vision and trachoma in Ethiopia. Federal Ministry of Health of Ethiopia 2006.
- WHO Alliance for the Global Elimination of Trachoma by 2020. Eliminating Trachoma: Accelerating Towards 2020, 2016.
- Habtamu E, Wondie T, Aweke S, et al. Trachoma and Relative Poverty: A Case-Control Study. PLoS Negl Trop Dis 2015; 9(11): e0004228.
- Emerson PM, Cairncross S, Bailey RL, Mabey DCW. Review of the evidence base for the ‘F’ and ‘E’ components of the SAFE strategy for trachoma control. Tropical Medicine & International Health 2000; 5(8): 515-27.
- Wright HR, Turner A, Taylor HR. Trachoma and poverty: unnecessary blindness further disadvantages the poorest people in the poorest countries. Clinical & experimental optometry : journal of the Australian Optometrical Association 2007; 90(6): 422-8.
- Taylor HR, Burton MJ, Haddad D, West S, Wright H. Trachoma. The Lancet 2014.
- Habtamu E, Wondie T, Aweke S, et al. Impact of trichiasis surgery on daily living: A longitudinal study in Ethiopia. Wellcome open research 2017; 2: 69.
- Habtamu E, Wondie T, Aweke S, et al. The Impact of Trachomatous Trichiasis on Quality of Life: A Case Control Study. PLoS Negl Trop Dis 2015; 9(11): e0004254.
- World Health O. Future Approaches to Trachoma Control. Report of a Global Scientific Meeting. Geneva, 17-20 June 1996. Geneva: World Health Organization, 1997.
- World Health Organization. Global WHO alliance for the elimination of blinding trachoma by 2020. Progress report on elimination of trachoma, 2010. Weekly Epidemiological Record 2012; 87: 161-8.
- Habtamu E, Heggen A, Haddad D, Center EE, Courtright P. Using a case study approach to document ‘preferred practices’ in mass drug administration for trachoma. COMMUNITY EYE HEALTH JOURNAL 2014; 27(88).
- Habtamu E, Wondie T, Aweke S, et al. Posterior lamellar versus bilamellar tarsal rotation surgery for trachomatous trichiasis in Ethiopia: a randomised controlled trial. The Lancet Global Health 2016; 4(3): e175-e84.
- World Health Organization Alliance for the Global Elimination of Trachoma by 2020. Second Global Scientific Meeting on Trachomatous Trichiasis. Cape Town, South Africa, 4-6 November 2015.
Oumer Shafi Abdurahman and the Stronger-SAFE project have been featured in an article on the Huffington Post website. The article addresses the issue of trachoma in Ethiopia. You can read the article here.
The London School of Hygiene & Tropical Medicine is to lead a major new research project that aims to accelerate the elimination of trachoma.
Stronger-SAFE is a £3.9m Wellcome Trust funded project that will increase our understanding of how trachoma is transmitted, and hopefully lead to the development and testing of new, more effective interventions and treatment approaches. The five year study will take place in Ethiopia where the disease is highly endemic, and be conducted with partners the Ethiopian Ministry of Health, the Oromia Regional Health Bureau, The Fred Hollows Foundation, the Wellcome Trust Sanger Institute and Monash University in Australia.
Trachoma is an eye disease caused by infection with the bacterium Chlamydia trachomatis. Around 190 million people worldwide live in endemic areas and require treatment. After repeated eye infections, trichiasis develops, a condition where the eyelids turn inwards and the lashes scrape the surface of the eye, causing great pain and often leading to permanent loss of vision.
Trachoma is thought to spread through person-to-person contact and by flies that have been in contact with discharge from the eyes of an infected person. The disease is responsible for 3% of the world's blindness, with more than 80% of the burden of active trachoma concentrated in 14 Sub-Saharan African countries. Ethiopia is the most severely affected country.
To combat trachoma, the World Health Organization Alliance for the Global Elimination of Trachoma by 2020 (GET2020) recommends the SAFE Strategy: Surgery for trichiasis, mass distribution of the antibiotic Azithromycin to treat chlamydial infection, Facial cleanliness and Environmental improvement to suppress transmission. Many endemic countries are implementing SAFE, and there is a major effort to scale-up activities with the aim of eliminating trachoma as a public health problem by 2020.
However, data from hyperendemic regions, areas where trachoma rates are continually high such as Ethiopia, suggest that current approaches do not consistently have the anticipated impact on infection and disease. Antibiotic schedules are not achieving reliable long-term control after treatment is finished and the ‘F&E’ components, such as improving water access, sanitation and hygiene (WASH) and fly-control, are not clearly defined and inconsistently implemented. Detailed studies investigating potential transmission routes and their relative importance have never been conducted, a gap that Stronger-SAFE aims to address.
Matthew Burton, Professor of International Eye Health at the London School of Hygiene & Tropical Medicine, is the project’s Principal Investigator. He said: “Trachoma is a terrible disease. Of the 190 million people who live in areas where it’s endemic, around two million are visually impaired, of whom 500,000 are blind. Although there has been a concerted international effort to tackle the disease, with success in many regions, elimination in highly endemic regions by 2020 is less certain, with recent research suggesting that current methods to control trachoma in these regions aren’t as effective as previously thought.”
Stronger-SAFE involves three phases. The first will focus on understanding how trachoma is transmitted in households and communities. Observational studies will document hygiene practice, sleeping arrangements and human behaviour that could promote transmission, as well as evaluating the contribution of fly to eye contact. Working closely with affected communities, Phase 2 aims to develop new approaches to stop the spread of disease, informed by the results from Phase 1.
Phase 3 is a cluster randomised controlled trial. It will test whether a combination of a double-dose of antibiotics and the newly developed facial cleanliness and environmental improvement intervention package from Phase 2, will be more effective than current interventions in the elimination of trachoma.
Professor Burton said: “Trachoma is a disease of poverty that mainly affects people who live in hot, dry areas where there is poor availability of water and sanitation. New, comprehensive and robust research is urgently needed to support the development of more effective evidence-based strategies if we are to defeat it. Thanks to Wellcome, and working closely with project partners, Stronger-SAFE could provide answers to improve the quality of life for people who live in some of the poorest parts of the world.”
Stronger-SAFE will be conducted in Oromia, Ethiopia. Biruck Kebede, Acting Director, Disease Prevention and Control, Federal Ministry of Health, Ethiopia, said: "Trachoma is a catastrophic and costly disease for Ethiopia. With more than 70% of districts in Ethiopia currently requiring mass drug administration, more than 73 million people are affected by trachoma - almost 80% of the Ethiopian population.
“The Ethiopian government is committed to eliminating trachoma. Though we are seeing rewarding results we now stand at a point where we need to gather evidence for intensifying our interventions if we are to meet our GET2020 commitments and targets. We believe that Stronger SAFE will provide this much needed evidence that will enable Ethiopia to eliminate trachoma."
Anthony Solomon, Medical Officer in the World Health Organization’s Department of Control of Neglected Tropical Diseases, added: “Political commitment for trachoma elimination has never been stronger. The work that will be completed by the Stronger-SAFE partners will hopefully provide long-overdue answers to questions that are critically important for optimizing the strategies used by programmes for combatting this disease. These are landmark studies which will help accelerate the end of one of the world’s most unfair diseases.”
Erica Pufall, from Wellcome’s Population Health team said: “Neglected Tropical Diseases like trachoma have a devastating impact, hitting poorest communities hardest. Wellcome is committed to supporting research to better understand and to improve treatments of these diseases. We are delighted to support this study to help eliminate this painful, infectious disease and prevent millions of people losing their sight because of it.”