New cryptococcal meningitis treatment as good as current care with far fewer serious side effects
24 March 2022 London School of Hygiene & Tropical Medicine London School of Hygiene & Tropical Medicine https://lshtm.ac.uk/themes/custom/lshtm/images/lshtm-logo-black.png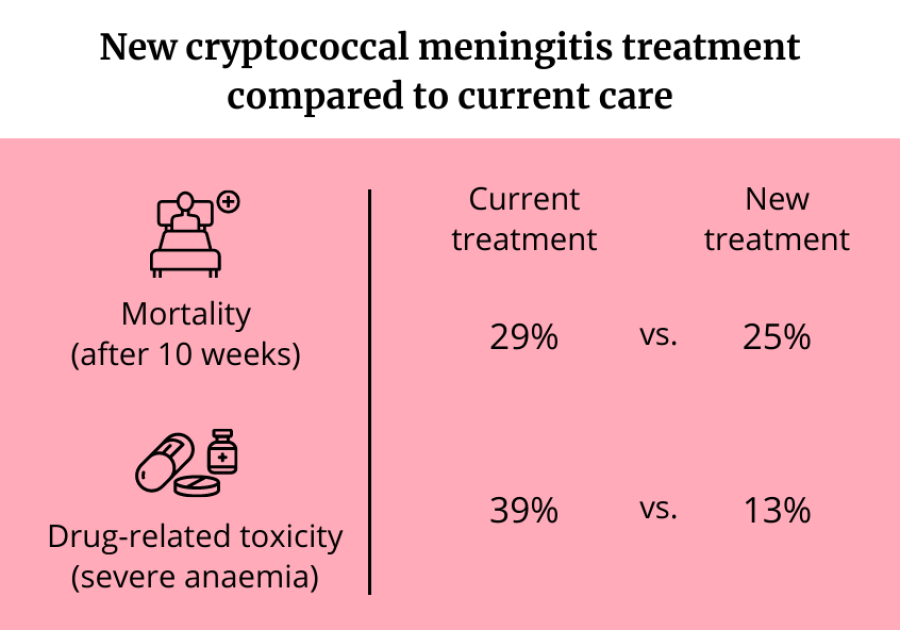
A new short course of treatment for HIV-associated cryptococcal meningitis is as effective at preventing deaths as the current longer recommended regimen but causes far fewer serious side effects, according to research in the New England Journal of Medicine.
The study involved a randomised trial in southern and eastern Africa and was conducted by an international research team, including scientists from the London School of Hygiene & Tropical Medicine, and partners in Botswana, France, Malawi, South Africa, Uganda, the United Kingdom and Zimbabwe.
The researchers say the new ‘one-dose’ approach offers a practical, easier-to-administer and better tolerated treatment for HIV-associated cryptococcal meningitis in Africa with the potential to reduce the length and cost of hospital admissions.
Cryptococcal meningitis is a fungal infection that affects the brain, and causes a serious disease in immunosuppressed people living with HIV across the globe. There are around 180,000 cryptococcal meningitis-related deaths each year, the majority of which occur in sub-Saharan Africa. Current treatments are either a 7 or 14-day course of amphotericin-B, combined with either oral antifungal tablets or oral fluconazole.
This new trial, the largest of its kind, investigated whether a single high dose of liposomal amphotericin-B (L-AmB, Ambisome) paired with two oral antifungals, fluconazole and flucytosine, was as effective at reducing deaths as the currently recommended WHO first-line treatment based on seven days of Amphotericin-B therapy.
Dr Melanie Alufandika-Moyo, study author and the lead research doctor at the Malawi-Liverpool Wellcome Unit, said: “Cryptococcal meningitis is the most common type of adult meningitis in much of Africa. Without effective treatment, infection progresses quickly, often resulting in deaths. Current treatment requires prolonged hospitalisation, intensive nursing care and costly laboratory monitoring which can be expensive for the healthcare system and the patient. Amphotericin-B can also cause kidney damage and blood problems.
“We urgently need new ways of treating the disease, so it’s fantastic that we were able to show a new streamlined treatment, requiring just one intravenous infusion, is as effective and less dangerous for patients.”
More than 800 adult patients with a first episode of HIV-associated cryptococcal meningitis, from five countries in southern and eastern Africa, took part in the trial.
Half received the new intervention (AmBisome arm), and half received the current recommended standard care (control arm). After 10 weeks, 25% (101/407) of people in the AmBisome arm died compared to 29% (117/407) in the control arm - this is among the lowest mortality rate reported from a major cryptococcal meningitis trial in Africa, despite more than a quarter of participants presenting with very severe disease.
As well as being as effective at saving lives, drug-related toxicity was significantly lower in the new ‘one-dose’ AmBisome arm. Anaemia occurred in 13% of AmBisome participants compared to 39% in the control arm. More participants in the control arm needed blood transfusions. There was also a difference in the impact on kidney function with far less drug related kidney toxicity in the one dose AmBisome arm than in the control arm.
AmBisome, a liposomal formulation of amphotericin-B, was suspected to be an effective cryptococcal meningitis treatment as it is less toxic and can be given in large doses that remain in the brain for some time. Previous work had found that a single, high-dose of AmBisome was effective at clearing Cryptococcus from around the brain - the catalyst for this new trial which tested AmBisome’s impact on a large number of patients in real-world settings.
Professor Tom Harrison from St George’s, University of London, who co-led the trial with Professor Joe Jarvis from the London School of Hygiene & Tropical Medicine and Botswana Harvard AIDS Institute Partnership, said: “These exciting results represent the culmination of a long programme of collaborative work to optimise antifungal drug combinations and reduce deaths from this terrible infection, and provide the strong evidence needed for policymakers to decide how cryptococcal meningitis should be treated going forward.
“Fortunately, with the support of advocates and funders, Ambisome and flucytosine are now becoming more available, which is essential to enable wide-scale implementation of this novel treatment regimen.”
Professor Joe Jarvis, the lead author of the study, said: “The results of this trial have the potential to transform how cryptococcal meningitis is treated and the management of advanced HIV-related disease in sub-Saharan Africa. It has far fewer significant side effects, which is obviously hugely important, and has the potential to prevent a large number of deaths in low-resource settings by being both easier to administer and cost-effective.”
The authors acknowledge limitations of the study, including the current lack of access to Ambisome and flucytosine, the key components of this novel treatment regimen, in many low-resource settings. To address this, Professor Jarvis and Dr David Lawrence, lead clinician on the trial, have recently been awarded a further five years of funding from the US Centers for Disease Control and Prevention (CDC) to help implement the study findings. They will work with the research teams in Botswana, Malawi, Uganda, and Zimbabwe to ensure that the novel treatment regimen reaches the patients who need it most.
The study was conducted by the London School of Hygiene & Tropical Medicine, St George’s, University of London, the Infectious Diseases Institute at Makerere University, Kampala, Uganda, the Malawi-Liverpool Wellcome Trust Clinical Research Unit, University of North Carolina Project in Malawi, University of North Carolina Project in Malawi, the University of Cape Town in South Africa, the Botswana-Harvard AIDS Institute Partnership, and the University of Zimbabwe, with European partners at the Liverpool School of Tropical Medicine and University of Liverpool, and the Institut Pasteur in Paris.
The study was funded by the European and Developing Countries Clinical Trials Partnership (EDCTP2) supported by the European Union (grant number TRIA2015-1092), the Swedish International Development Cooperation Agency, and the UK Department of Health and Social Care, the UK Foreign Commonwealth and Development Office, the UK Medical Research Council and Wellcome Trust, through the Joint Global Health Trials scheme.
Publication
J.N. Jarvis, D.S. Lawrence et al. Single-Dose Liposomal Amphotericin B Treatment for Cryptococcal Meningitis. The New England Journal of Medicine. DOI:10.1056/NEJMoa2111904
If you enjoyed this article and would like to build a career in global health, we offer a range of MSc programmes covering health and data, infectious and tropical diseases, population health, and public health and policy.
Available on campus or online, including flexible study that works around your work and home life, be part of a global community at the UK's no.1 public health university.